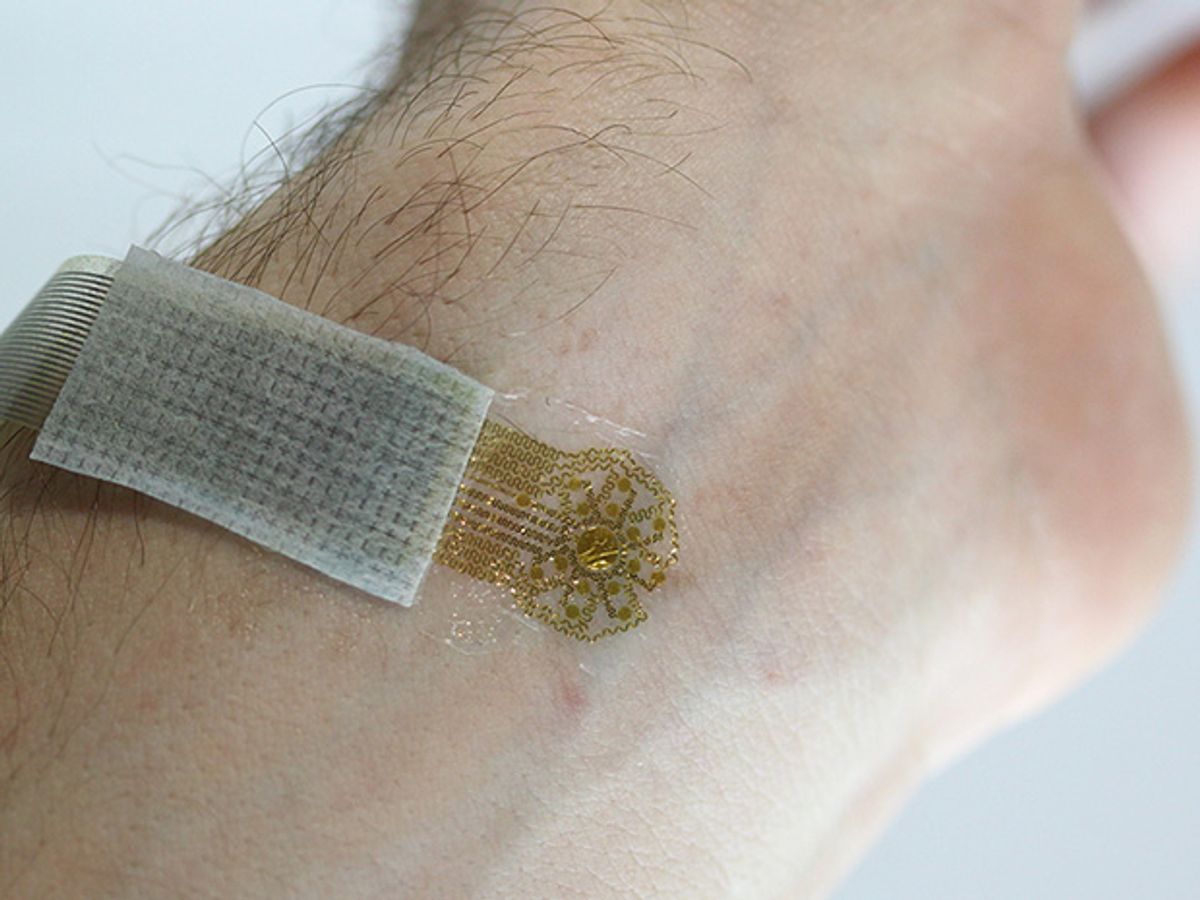
Today’s best medical devices for measuring blood flow require patients to first show up at a clinic or hospital, then stay very still during the imaging procedure. But an experimental sensor that clings to skin like a temporary tattoo could enable 24-hour monitoring of blood flow wherever a patient goes.
A wearable sensor could mean the difference between taking what is essentially a snapshot of a patient’s health while he or she is at the clinic, and getting the equivalent of around-the-clock video of that person’s blood flow throughout the day. Testing showed that a flexible “epidermal electronics” blood flow monitor developed by an international team led by researchers at the University of Illinois at Urbana-Champaign can measure the blood flow in the outermost 1 to 2 millimeters of skin—even for human bodies in motion. That points to the possibility of a future wearable device that could continuously measure the blood flow of patients while they go about their daily lives.
“Say you have diabetic patients and want to be able to monitor changes in specific blood vessels continuously for 24 hours a day,” says Richard Chad Webb, a Ph.D. candidate in materials science and engineering at the University of Illinois. “There’s no way of doing that today.”
The University of Illinois team developed the new wearable device in cooperation with the U.S. National Institutes of Health and a broader group of U.S. and Chinese researchers. Webb was the lead author of a paper detailing the group’s work; it was published in the 30 Oct 2015 online issue of the journal Science Advances.
Most state-of-the-art devices for measuring blood flow use optical imaging techniques that require patients to stay still during the process. Webb and his colleagues turned to flexible electronics technology to find a possible wearable solution. (One of the study’s coauthors is John Rogers, a materials scientist and engineer at the University of Illinois whose lab has pioneered many examples of biocompatible flexible electronics.)
Researchers eventually developed a lightweight, ultra-thin device that sits on top of the skin without distorting the blood flow it seeks to measure. It clings tightly to the skin due to van der Waals forces—the weak attractive forces between molecules. This attraction prevents any motion between the sensor and skin that could affect the accuracy of readings. As a backup, medical tape can ensure the device stays put.
“Fundamentally, what we were trying to do was remove the relative motion between the body and detector system,” Webb explains. “That allows you to get to same clinical information [as state-of-the-art optical imaging devices] without the restriction of immobilizing somebody.”
Webb and his colleagues built the device from ultra-thin layers of silicon, gold, chromium, and copper supported by silicone. Most of the sensor’s bulk comes from a 40-micrometer-thick layer of silicone. Each of the other layers has a thickness of just tens or hundreds of nanometers.
The wearable gadget detects differences in heat patterns caused by the blood flow beneath the skin. A 1.5-millimeter thermal actuator within the device heats up by 6 to 7 degrees Celsius to provide a thermal background for the measurements. That sounds like a significant temperature change for something sitting against human skin, but it’s below the threshold of skin sensitivity. The 3.5 milliwatts per square millimeter of thermal energy entering the skin is so minuscule that someone wearing the device wouldn’t notice the difference.
Two rings of sensors around the actuator detect the temperature differences in the heat patterns with a precision within 0.01 degrees Celsius. Last but not least, computer algorithms help interpret the heat pattern differences as blood flow rate.
Testing with the wearable device placed above the wrist veins of human volunteers showed how it could work in practice. Blood flow measurements were taken as the human subjects stood motionless for five minutes, as they stepped up and down on an aerobic stepper for three minutes, and, finally, as they lied down on their backs. Researchers also compared the wearable device’s results with the state-of-the-art optical imagers to ensure that the measurements were reasonably accurate.
There’s still a ways to go before this experimental device could lead to a commercial wearable. The researchers still need to figure out how to make a version complete with a self-contained power source and components that would let it wirelessly transmit data to a laptop or other device, says Webb.
But once that happens, such devices could help revolutionize medicine by providing an unprecedented amount of data for understanding health conditions such as diabetes, the hardening of arteries, and general human aging. Such flexible sensors could also be placed on internal organs, surgical tools, or implantable devices.
For now, Webb and his colleagues continue to refine the heat-mapping blood flow device with the goal of making it smaller. A next step might be the development of a device that could measure blood flow through individual capillaries rather than within just the larger blood vessels.
Jeremy Hsu has been working as a science and technology journalist in New York City since 2008. He has written on subjects as diverse as supercomputing and wearable electronics for IEEE Spectrum. When he’s not trying to wrap his head around the latest quantum computing news for Spectrum, he also contributes to a variety of publications such as Scientific American, Discover, Popular Science, and others. He is a graduate of New York University’s Science, Health & Environmental Reporting Program.