Counterfeit malariamedications can easily fool the eye: The fake drugs sold in markets throughout Africa and Asia often look exactly like the authentic products. The pills are the right shape and size, the packaging is identical to that of the real brand, and the boxes often feature the duplicated logos and holographic stickers of official regulators.
But these knockoffs can’t fool chemistry. That’s why engineers from Global Good, a philanthropic invention lab in Bellevue, Wash., are trying to solve the counterfeit problem with a handheld device that uses optical spectrometry to check the chemical composition of medications. In the next few months, drug inspectors and pharmacists in Kenya, Namibia, and Laos will begin field trials of the technology.
The researchers foresee “a top-down path to adoption,” says Ben Wilson, the project’s lead investigator. Global Good is funded by Bill Gates and the Bellevue-based innovation hub Intellectual Ventures, and it benefits from well-established partnerships with government ministries of health and international aid groups. “If our field trials go well, the technology could be used on a country level next year,” Wilson says.
Counterfeit drugs are a huge problem in the developing world, and antimalarials are a particular source of concern. “The active ingredient in antimalarials is the biggest cost, so by leaving it out, the counterfeiter can make a better margin on the pills,” Wilson explains. A 2012 survey published in The Lancet Infectious Diseases found that 35 percent of 3,700 drug samples tested in Southeast Asia and sub-Saharan Africa were either fake or of poor quality.
The new system uses near-infrared (NIR) spectrometry, directing a beam of NIR light at a pill and recording how the light is absorbed. That pattern of absorption is a unique spectral signature that reveals the chemical composition of the pill without damaging it. Until recently, NIR spectrometry required bulky and expensive tools that limited it to fields like astronomy and medical imaging. But rapid advances in the technology have led to cheap and miniaturized devices that enable new applications.
The researchers from Global Good first built a smartphone app that worked with SCiO, a handheld infrared spectrometer that recently came on the market for consumers and businesses. In one proof-of-concept experiment, which they reported in The American Journal of Tropical Medicine and Hygiene, the researchers tested 77 brands of antimalarial drugs purchased in Equatorial Guinea and 31 bought in Ghana. The app contained a library of the appropriate spectral signatures for each of those brands, and the researchers found that the software was able to reliably distinguish between authentic and fake pills. But the SCiO required that the smartphone be connected to the cloud for analysis of the medicine, which Wilson says isn’t always possible in remote towns and health clinics. So, his team switched out the hardware and is now working with a handheld NIR spectrometer made by the Taiwanese company Young Green Energy Co.
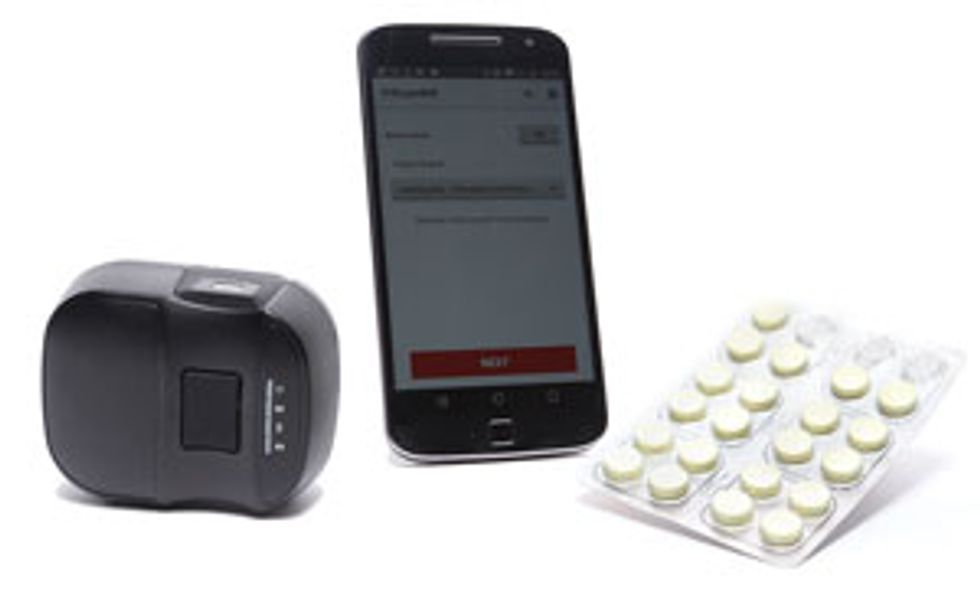
The new system hosts all the analysis locally on a smartphone. With the Global Good app, developed for both iOS and Android phones, the user inputs the brand of medication that’s being checked and hits the scan button. Two seconds later, the system gives an answer: The app shows the spectral signature of the pill and states whether or not it’s authentic.
In the 2012 Lancet study on antimalarials, the authors wrote that “production and distribution of counterfeit antimalarial drugs should be prosecuted as crimes against humanity.” The lead author of that report, Gaurvika Nayyar, says fake malaria meds cause thousands of deaths in countries where malaria is epidemic, and they particularly affect young children.
Nayyar, a consultant who serves as an advisor at the Global Health Policy Institute in San Diego, recently reviewed new technologies used to combat fake drugs. She says there is a need for low-power portable devices that don’t require much user training, as such devices could be used by pharmacists or patients themselves to check their medications. But she also sees value in more systemic approaches, such as using RFID tags or blockchain technology to track authentic medications from factory to pharmacy. “I think we need a clear comparative assessment of the various emerging technologies to find out which ones work for which parts of the supply chain,” she says. “There’s no one solution that will solve the problem.”
When Global Good set out to develop a tool for the fight against fake drugs, Wilson says his team considered all the ways counterfeiters could game the system, including setting up fake websites that “verify” fake meds. They decided to develop a technology using NIR spectrometry because it’s so hard to spoof; trying to match the spectral signature of a pill would be an expensive proposition, he says. “For the counterfeiter, it would probably be cheaper to just put the active ingredient in.”
This article appears in the August 2017 print issue as “Fake Malaria Meds Meet Their Match.”
This article was updated on August 4, 2017.
