Three research groups taking very different approaches to building an artificial kidney all have the same goal: giving people with kidney failure an escape from today’s dialysis routine. Dialysis keeps people alive, but it’s also pretty terrible.
A typical patient goes to a clinic three times each week to be hooked up to a dialysis machine, then lies there for 3 or 4 hours while blood cycles out of the body, through the machine, and back in again. The machine substitutes for working kidneys by filtering out toxic waste products, maintaining the balance of electrolytes, and removing excess water.
In addition to losing time and mobility, most patients have to carefully restrict their diet and fluid intake to stay healthy between sessions. Patients also deal with a host of side effects, says Steven Weisbord, a kidney specialist at the University of Pittsburgh School of Medicine. His studies have documented downsides that include extreme fatigue, depression, low blood pressure, and muscle cramps. “It is a lifeline for patients,” Weisbord says, “but [dialysis] is associated with significant decrements in quality of life and bothersome symptoms.”
Here are three ideas that might lead to a better way.
The Wearable Artificial Kidney showed promising results in a recent clinical trial.Photo: Stephen Brashear
Kidney-on-a-Belt
The wearable artificial kidney, or WAK, looks rather like a bulky utility belt. In a recent clinical trial, patients wore the WAK for 24 hours of continuous treatment, with mixed results. Technical problems halted the study early, but the inventors say those problems are fixable, and they stress that the device provided both effective treatment and a better quality of life for the test subjects.
In typical dialysis machines, blood flows into a tube called the dialyzer, where waste particles pass through a membrane into a solution that carries them away. Fresh solution continuously flows into the dialyzer. On the 5-kilogram WAK belt, the solution cycles through a miniature dialyzer and then back to cartridges where the toxins are absorbed so the solution can be cycled through again.
During the 24-hour test, conducted by researchers at the University of Washington and the University of California, Los Angeles, the battery-powered wearable device cleared toxins from the blood as effectively as a typical dialysis machine does.
The trial subjects’ experience suggests that the WAK can improve quality of life, as they could walk around or sleep during treatment. They could also eat and drink whatever they wanted, unlike ordinary dialysis patients.
However, the technical problems were significant: The trial’s seven participants encountered kinked tubes, an erratic pump, and batteries and absorbent cartridges that needed replacing. Most important, gas bubbles were found in the WAK’s solution circuit, which can be deadly if they reach the heart or brain. The device includes bubble alarms and degassing vents, but the researchers plan a redesign to reduce gas production and improve venting.
The WAK will have to operate flawlessly to fulfill the ultimate goal stated in the researchers’ journal article in JCI Insight: “for treatment with the WAK to be self-administered independently by patients and caregivers in the home environment.”
A hybrid device would use both mechanical and biological components.Illustration: The Kidney Project
The Cyborg Kidney
Researchers from the University of California, San Francisco, and the Cleveland Clinic, in Ohio, started the Kidney Project in 1998 to build a “bioartificial” kidney that combines mechanical and biological parts.
The implantable device is about the size of a coffee cup. Blood first flows into a filtering unit that draws waste particles and other molecules through a silicon membrane; that resulting slurry then passes through a bioreactor unit containing live kidney cells that sends sugars and salts back to the blood. The cells inside the bioreactor cartridge come from donated kidneys not suitable for transplant.
Researchers haven’t yet tested an entire prototype of their cyborg kidney, but trials of the individual units have been promising. One study tested the bioreactor on patients in the intensive-care unit with life-threatening acute kidney injuries. Half the patients had their blood cycled through a dialyzer alone, while the other half’s blood went through both a dialyzer and an external bioreactor unit. The control group’s survival rate (measured 180 days later) was 39 percent, while the bioreactor group’s rate was 67 percent.
The Kidney Project is actively soliciting funding to reach its goal—a commercial device that offers “a cure rather than a treatment.” Last year the U.S. National Institutes of Health gave the researchers a US $6 million grant to push toward clinical trials, which they hope to start in late 2017.
The startup Qidni recently tested its prototype in a living pig with no renal function.Photo: Qidni
The Implant
The third contender comes from a young startup that recently received an investment from IndieBio, a San Francisco accelerator for biotech companies. Qidni Labs is building a fully implantable artificial kidney that uses a nanofiltration system to mimic the organ’s function, even going so far as to drain waste products into the bladder. Company founder Morteza Ahmadi will divulge only the basics about his hardware, but he says his prototype performed well when implanted in pigs in July.
Ahmadi began working on miniaturized dialysis systems in 2010 as a Ph.D. student at the University of Waterloo, in Ontario, Canada. Like the researchers behind the Kidney Project, he decided to make a blood filter from ultrathin membranes of crystalline silicon. Thanks to manufacturing techniques perfected in the semiconductor industry, such silicon membranes can be mass produced with pore sizes ranging from 5 to 20 nanometers—big enough to allow waste particles through, yet too small for blood cells.
In a 2013 paper, Ahmadi and his colleagues noted that this ultrathin crystalline silicon is challenging to work with because it’s prone to fracture. Also, as silicon can provoke an immune reaction, the membrane must be coated with a biocompatible material. Ahmadi won’t say how his design team solved these problems, or how the fully implantable device will be powered. But he claims the device will continuously filter the patient’s blood for years without requiring maintenance or cleaning, thus achieving his goal: “The idea is to free patients from dialysis machines forever,” he says.

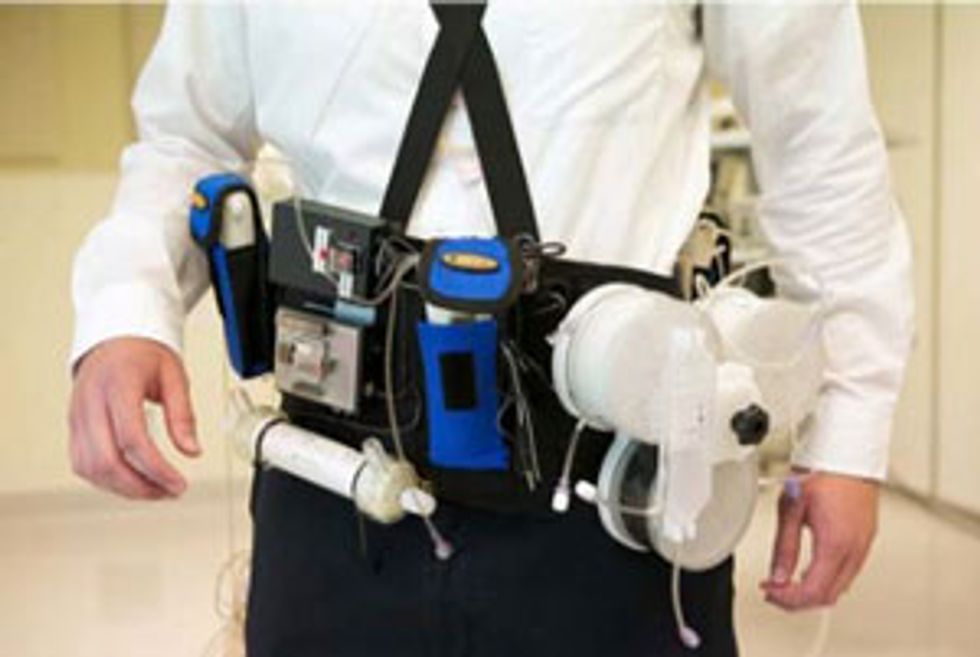 The Wearable Artificial Kidney showed promising results in a recent clinical trial.Photo: Stephen Brashear
The Wearable Artificial Kidney showed promising results in a recent clinical trial.Photo: Stephen Brashear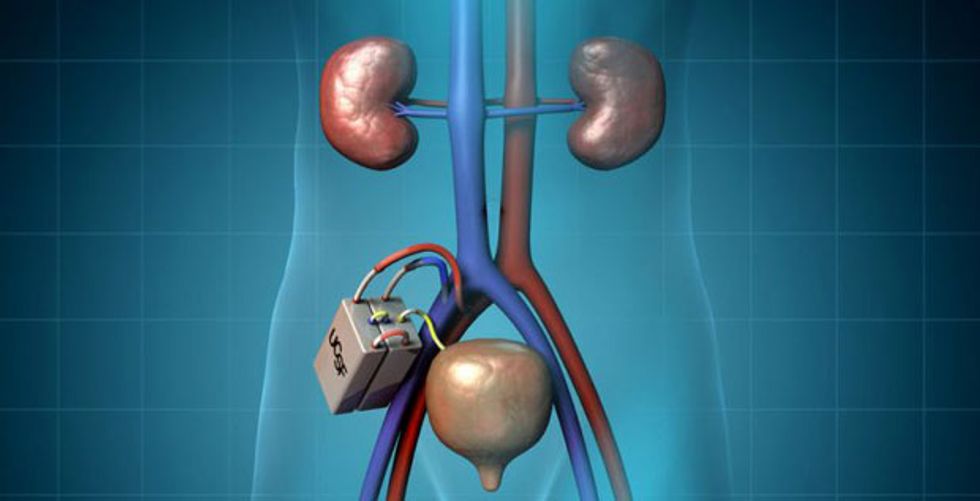 A hybrid device would use both mechanical and biological components.Illustration: The Kidney Project
A hybrid device would use both mechanical and biological components.Illustration: The Kidney Project The startup Qidni recently tested its prototype in a living pig with no renal function.Photo: Qidni
The startup Qidni recently tested its prototype in a living pig with no renal function.Photo: Qidni