Sweat: We all do it. It plays an essential role in controlling body temperature by cooling the skin through evaporation. But it can also carry salts and other molecules out of the body in the process. In medieval Europe, people would lick babies; if the skin was salty, they knew that serious illness was likely. (We now know that salty skin can be an indicator for cystic fibrosis.)
Scientists continue to study how the materials in sweat can reveal details about an individual’s health, but often they must rely on gathering samples from subjects during strenuous exercise in order to get samples that are sufficiently large for analysis.
Now researchers in China have developed a wearable sensor system that can collect and process small amounts of sweat while providing continuous detection. They have named the design a “skin-interfaced intelligent graphene nanoelectronic” patch, or SIGN for short. The researchers, who described their work in a paper published in Advanced Functional Materials, did not respond to IEEE Spectrum’s interview requests.
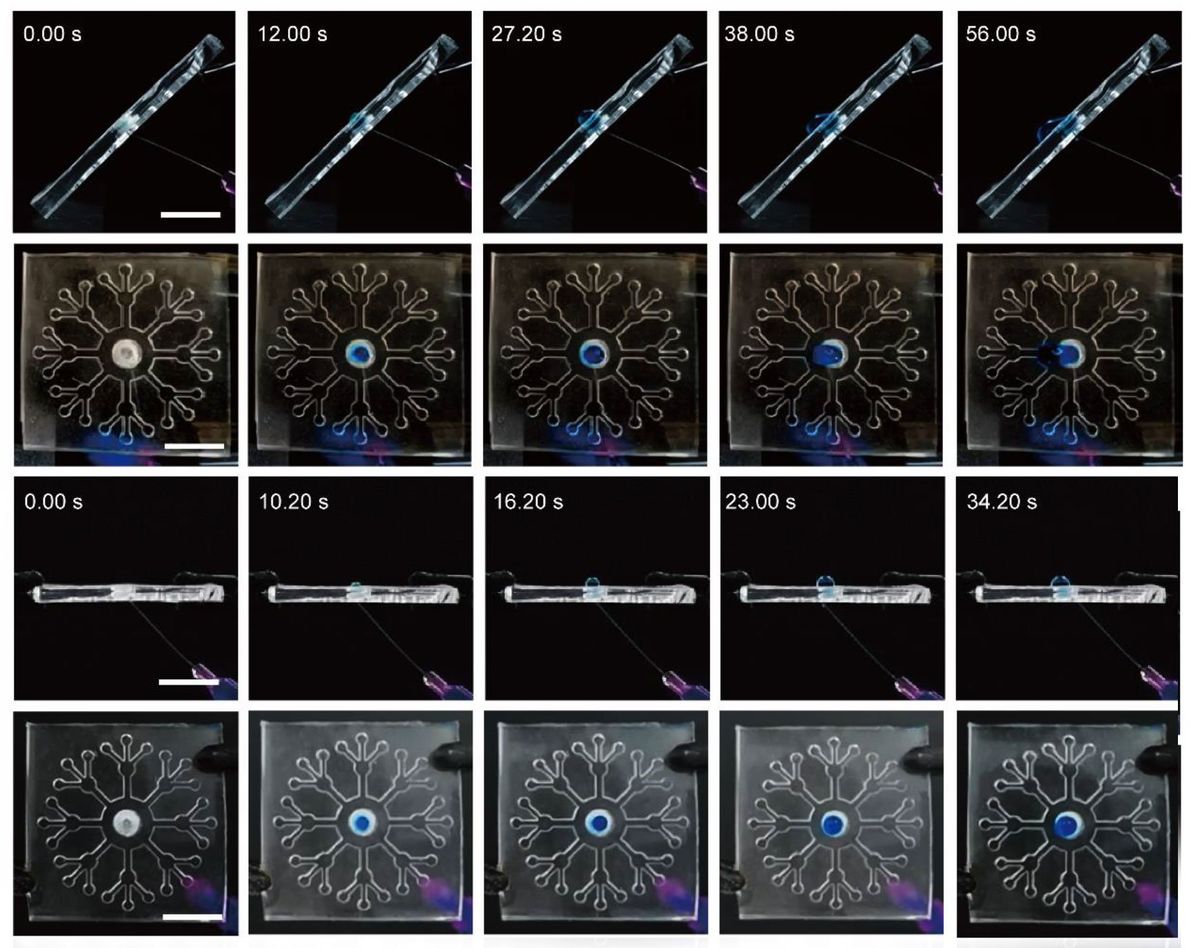
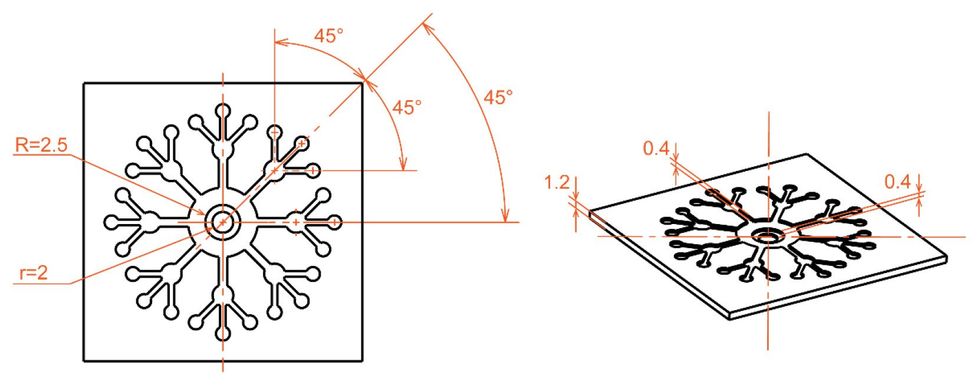
The SIGN sensor patch relies on three separate components to accomplish its task. First, the sweat must be transported from the skin into microfluidic chambers. Next, a special membrane removes impurities from the fluid. Finally, this liquid is delivered to a bioreceptor that can be tuned to detect different metabolites.
The transport system relies on a combination of hydrophilic (water-attracting) and hydrophobic (water-repelling) materials. This system can move aqueous solutions along microchannels, even against gravity. This makes it possible to transport small samples with precision, regardless of the device’s orientation.
The fluid is transported to a Janus membrane, where impurities are blocked. This means that the sample that reaches the sensor is more likely to produce accurate results.
Finally, the purified sweat arrives at a flexible biosensor. This graphene sensor is activated by enzymes designed to detect the desired biomarker. The result is a transistor that can accurately measure the amount of the biomarker in the sample.
One interesting feature of the SIGN patch is that it can provide continuous measurements. The researchers tested the device through multiple cycles of samples with known concentrations of a target biomarker, and it was about as accurate after five cycles as it was after just one. This result suggests that it could be worn over an extended period without having to be replaced.
Continuous measurements can provide useful longitudinal data. However, Tess Skyrme, a senior technology analyst at the research firm IDTechEx, points out that continuous devices can have very different sampling rates. “Overall, the right balance of efficient, comfortable, and granular data collection is necessary to disrupt the market,” she says, noting that devices also need to optimize “battery life, calibration, and data accuracy.”
The researchers have focused on lactate—a metabolite that can be used to assess a person’s levels of exercise and fatigue—as the initial biomarker to be detected. This function is of particular interest to athletes, but it can also be used to monitor the health status of workers in jobs that require strenuous physical activity, especially in hazardous or extreme working conditions.
Not all experts are convinced that biomarkers in sweat can provide accurate health data. Jason Heikenfeld, director of the Novel Device Lab at the University of Cincinnati, has pivoted his research on wearable biosensing from sweat to the interstitial fluid between blood vessels and cells. “Sweat glucose and lactate are way inferior to measures that can be made in interstitial fluid with devices like glucose monitors,” he tells Spectrum.
The researchers also developed a package to house the sensor. It’s designed to minimize power consumption, using a low-power microcontroller, and it includes a Bluetooth communications chip to transmit data wirelessly from the SIGN patch. The initial design provides for 2 hours of continuous use without charging, or up to 20 hours in standby mode.
Alfred Poor is a technology speaker and writer with a focus on health tech. He was the editor of “Health Tech Insider,” a website that covered wearable and mobile devices for health and medical applications. He also helps tech company executives make a better impression in video meetings and online presentations. A graduate of Harvard College, he is the author or co-author of 15 books and is widely quoted in major media outlets.