19 December 2012—Years of studies to determine whether cellphones can cause brain tumors have yielded one popular consensus: More studies are needed. One important piece that has been missing from researchers’ arsenals is a way to see what happens to cellphone radiation that is absorbed by the human brain. Two scientists have now developed a magnetic resonance imaging (MRI) technique that they say could solve that problem. This could be an important tool for researchers who are trying to discover whether extensive cellphone use can cause brain tumors or other health problems.
The technique creates high-resolution 3-D images of the heat created by cellphone radiation absorbed in the brain. In research reported this week in Proceedings of the National Academy of Sciences, the scientists demonstrate the method on cow brain matter and a gel that emulates brain tissue. But the procedure could easily be adapted for tests on human brains, says David Gultekin, a medical physicist at Memorial Sloan-Kettering Cancer Center, in New York, who led the development of the technique.
Scientists generally agree that any harmful effects of radio frequency (RF) waves from cellphone antennas would arise from radiation heating up brain matter. Today, mapping that absorbed radiation involves measuring electric fields using probes that are inserted into dummy heads filled with gel. Computer simulations can also predict RF field distributions in the dummies. But those methods are indirect and too invasive to be used on people, Gultekin says. And they have low resolution, so they cannot map rapidly changing fields over tiny areas in the brain.
On the other hand, with adjustments to nuclear magnetic resonance (NMR)—the technology behind MRI—researchers should be able to directly make accurate 3-D maps of radiation-induced heat in real living human brains. “For the brain, you need a noninvasive technology. Nothing should penetrate the tissue,” Gultekin says. “NMR has that capability. It provides a 3-D temperature field with very high spatial and temporal resolution, and it can cover the whole head in less than 10 seconds.”
Doctors already use NMR to measure the degree to which tumors heat up during cancer thermal therapy. This involves placing atomic nuclei in a static magnetic field and then making them vibrate under an oscillating RF field to measure their resonance frequency. Heat changes the position of electrons that circle the nuclei of hydrogen atoms in the tissue. This changes the amount of magnetic field felt at the nuclei, altering their resonance frequency. The shift in frequency is proportional to temperature change.
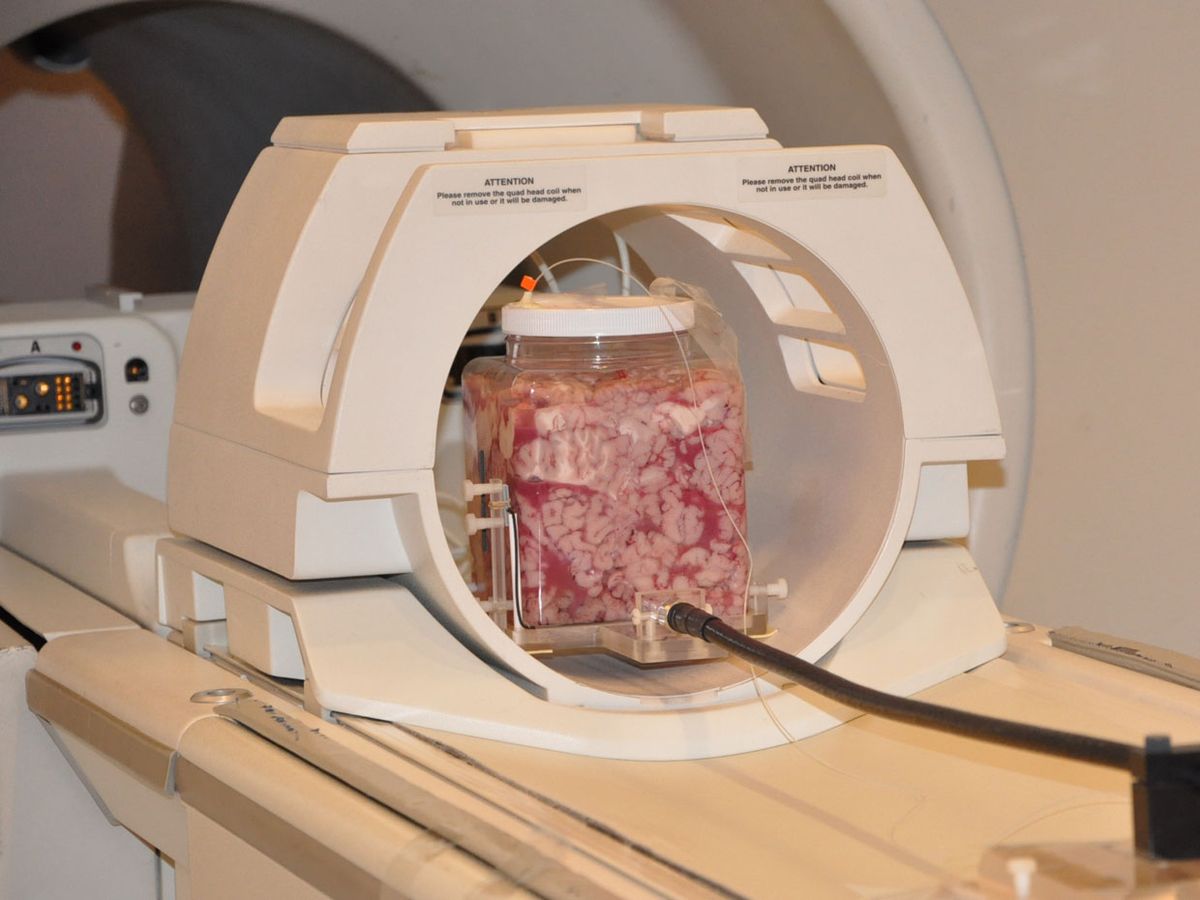
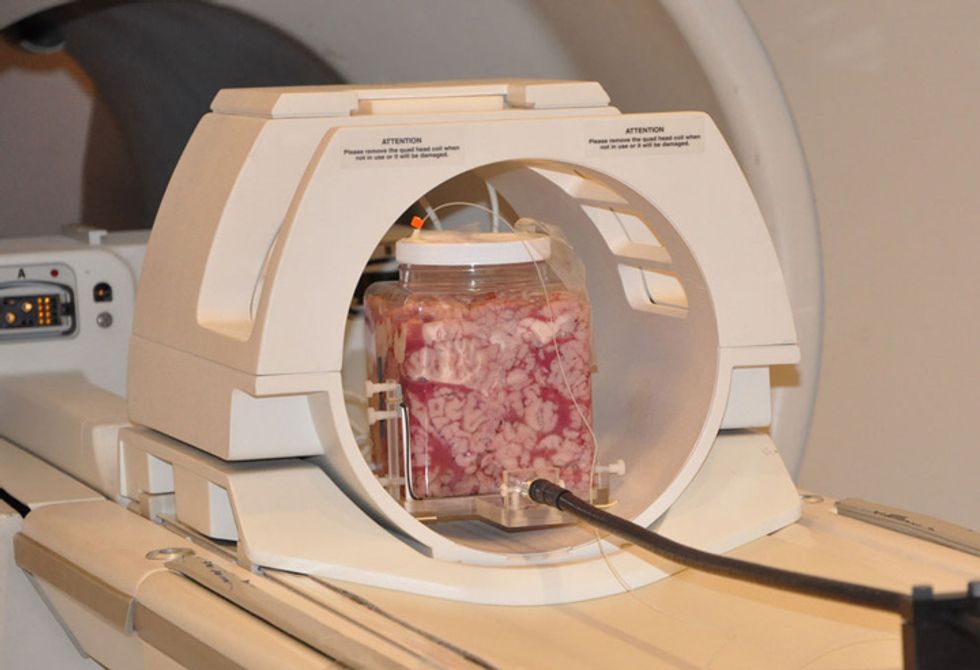
To generate 3-D heat maps of the brain, Gultekin and his colleague Lothar Moeller, an electrical engineer at Bell Laboratories (Alcatel-Lucent), in Holmdel, N.J., filled separate plastic containers with bovine brain tissue and gel. They couldn’t use a real cellphone handset in an MRI machine because the strong magnetic field would send it flying at deadly speed. So they fashioned an RF-emitting antenna made of a nonferromagnetic material.
One at a time, the researchers placed the sample containers with the antenna next to them in an MRI machine. They turned the antenna on for 12 minutes each at output powers of 125, 250, 500, 1000, and 2000 milliwatts—mimicking the range of typical cellphone outputs from average to peak power.
At 500 mW, 1 watt, and 2W, the temperature of the sample area closest to the antenna went up by 1, 3.5, and more than 5 °C, respectively. These increases showed up as hot spots in the 3-D images generated by the MRI machine. At 125 and 250 mW, the temperature changes were less than 1 °C and don’t appear in the images, but they can be calculated.
The researchers confirmed the temperature change with fiber-optic temperature sensors inserted in the samples. The MRI machine’s oscillating RF field also can heat up the samples, creating interfering signals, which the researchers screen out with filters in the frequency-detection circuit.
Kenneth Foster, a bioengineering professor at the University of Pennsylvania, calls the study “innovative” but questions its use for cellphone research , because of its low sensitivity. “In living brain tissue, there is a lot of blood flow that carries away heat, so actual temperature increases are very small,” he says. Nevertheless, he says, at its current sensitivity, the technique would be useful for safety studies of exposure to MRI and cancer heat and radiation therapy.
Gultekin says he is now optimizing the method for live brain measurements at low cellphone power levels and that it “could be as sensitive as required for living brain tissue.”
“I think it’s a very clean, clever idea,” says William Happer, a physics professor at Princeton University. Because NMR is noninvasive and commonly used in medicine already, Happer believes it should be easy to gain approval for using the technique on lab animals, and eventually humans, in order to study the effects of cellphone radiation.
About the Author
Prachi Patel is a contributing editor to IEEE Spectrum. In the September 2012 issue, she reported on the technology needed to monitor and forecast drought. You can also hear her on Spectrum Radio and Public Radio International’s “ Living on Earth.”