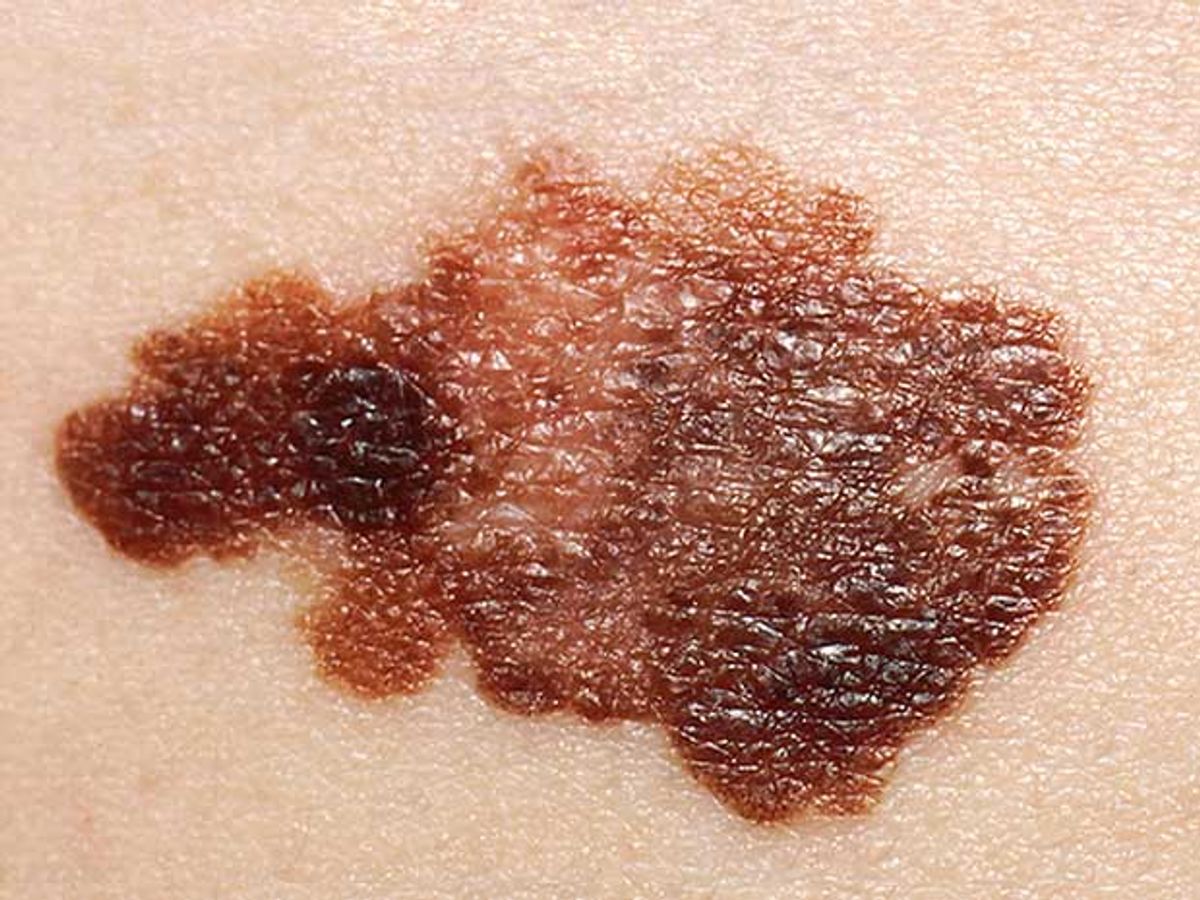
Researchers have developed an algorithm that recognizes skin cancer in photos about as well as dermatologists do. So says a study published today in Nature. The algorithm, developed by a group at Stanford University, is not the first automated system for recognizing skin lesions, but it’s likely the most robust, the researchers say.
“This is like when a computer first beat the world champion chess player,” says Sancy Leachman, a dermatologist and researcher at Oregon Health & Science University who was not involved in the study. Stanford’s program beat dermatologists—essentially the world champions of skin cancer diagnostics, she says. “That’s pretty cool.”
The study highlights the potential for artificial intelligence (AI) to enable anyone with a smartphone to have access to health care. “We’re working towards extending the reach of care outside of the clinic,” says Andre Esteva, the electrical engineering PhD student at Stanford who led the study.
Stanford built its deep learning algorithm on the architecture of the GoogleNet Inception v3, a convolutional neural network algorithm. Such programs are structured in interconnected layers that are inspired, at a high level, by the way neurons in the brain work.
Inception v3 was trained on 1.28 million images from the 2014 ImageNet Large Scale Visual Recognition Challenge, a contest that aimed to improve a computer’s ability to detect and classify objects in images. Stanford researchers then fine-tuned the algorithm with a set of nearly 130,000 images of skin lesions from more than 2000 diseases—the largest dataset used for automated skin cancer classification.
In the study, the algorithm went head-to-head against 21 board-certified dermatologists. The doctors reviewed hundreds of images of skin lesions, and for each one, determined whether they would conduct further tests on it or assure the patient that it was benign. The algorithm reviewed the same images and gave its diagnoses. Neither the doctors nor the algorithm had seen the images previously.
The computer performed on par with the experts. For example, the program was able to distinguish between keratinocyte carcinomas—the most common human skin cancer—and benign skin growths called seborrheic keratoses.
Stanford’s program will need to be subjected to tougher cases before it’s ready for the real world. The researchers didn’t ask the algorithm to distinguish, for example, between seborrheic keratoses and melanomas, which can be tough to do, says Leachman.
And since the dermatologists had to base their determinations solely on photos, it’s unclear whether the computer could match their expertise in clinical settings, where they could physically examine the lesions and read the patients’ medical histories. “Touch has a role,” says Leachman.
If the algorithm proves itself in the real world, there’s a huge upside, says Leachman. “The [medical] system is loaded up with people who don’t need to be seen,” she says. A computer that can sift through those cases would allow patients who really do need to be seen by a doctor to do so more quickly and effectively, she says.
It’s likely that not all dermatologists will welcome the intrusion of AI into their profession. “I think you’ll find a full spectrum of impressions,” says Leachman.
On one end, there will be some who fear machines taking over their jobs, she says. And there are many who are already skeptical of a computer’s ability, particularly the less robust, online diagnostics apps. IBM’s supercomputer Watson beat top Jeopardy players, but didn’t fare as well against doctors in making medical and diagnostic decisions.
At the other end, there will be doctors who think the technology opens up opportunities to use their time in ways that advance the field, Leachman says. She falls on the latter end of that spectrum. “Lets spend our time and brain power on something that hasn’t yet been solved,” and leave what we already know to the computers, she says.
Emily Waltz is a features editor at Spectrum covering power and energy. Prior to joining the staff in January 2024, Emily spent 18 years as a freelance journalist covering biotechnology, primarily for the Nature research journals and Spectrum. Her work has also appeared in Scientific American, Discover, Outside, and the New York Times. Emily has a master's degree from Columbia University Graduate School of Journalism and an undergraduate degree from Vanderbilt University. With every word she writes, Emily strives to say something true and useful. She posts on Twitter/X @EmWaltz and her portfolio can be found on her website.