Letting a snake-like robot glide into your mouth and down your throat may sound a bit alarming. Letting such a robot glide into any of your other orifices may sound more alarming still.
But the Flex Robotic System from Medrobotics, in Raynham, Mass., has earned high praise from a head and neck surgeon who has sent it snaking down 19 of his patients’ throats as of today. “It really is changing the way I do business,” says David Goldenberg, director of otolaryngology surgery at the Penn State Hershey Medical Center. “It is the future of head and neck surgery.” His surgical colleagues in the colorectal and OB-GYN departments are also planning clinical trials using the Flex, Goldenberg told IEEE Spectrum.
The Flex entered the U.S. market just last year (and the European market the year before that), and getting it approved by regulators was no easy task, Medrobotics executives told Spectrum. Interestingly, the biggest hassle was ensuring that the robot was dumb enough to meet the U.S. Food and Drug Administration’s (FDA’s) requirements.
“When we approached the FDA, almost the first question out of their mouth was about the autonomous nature of the robot. They raised it as a serious red flag,” says Medrobotics CEO Samuel Straface. “We had to show that the surgeon has complete and absolute control at all times. If it was any other way, we’d still be a science project,” he says.
This conjunction of statements from surgeon and CEO neatly sums up the current state of robotic surgery. The new “robots” coming out are giving surgeons new capabilities, but really they’re still just tools in the hands of the all-powerful human. That’s because the FDA has barred anything resembling an autonomous robotic assistant from the operation room.
Roboticists may see autonomous surgical bots as a grand research goal, as Spectrum explored recently in a feature article [Would You Trust a Robot Surgeon to Operate on You?]. And recent triumphs, like an autonomous system that stitched up pig intestines more effectively than human surgeons, have demonstrated their progress. But it’s a long way from the lab to the clinic, as Medrobotics discovered. “We’re injecting some reality,” says Straface. “Just because you can build these things doesn’t mean you can sell them.”
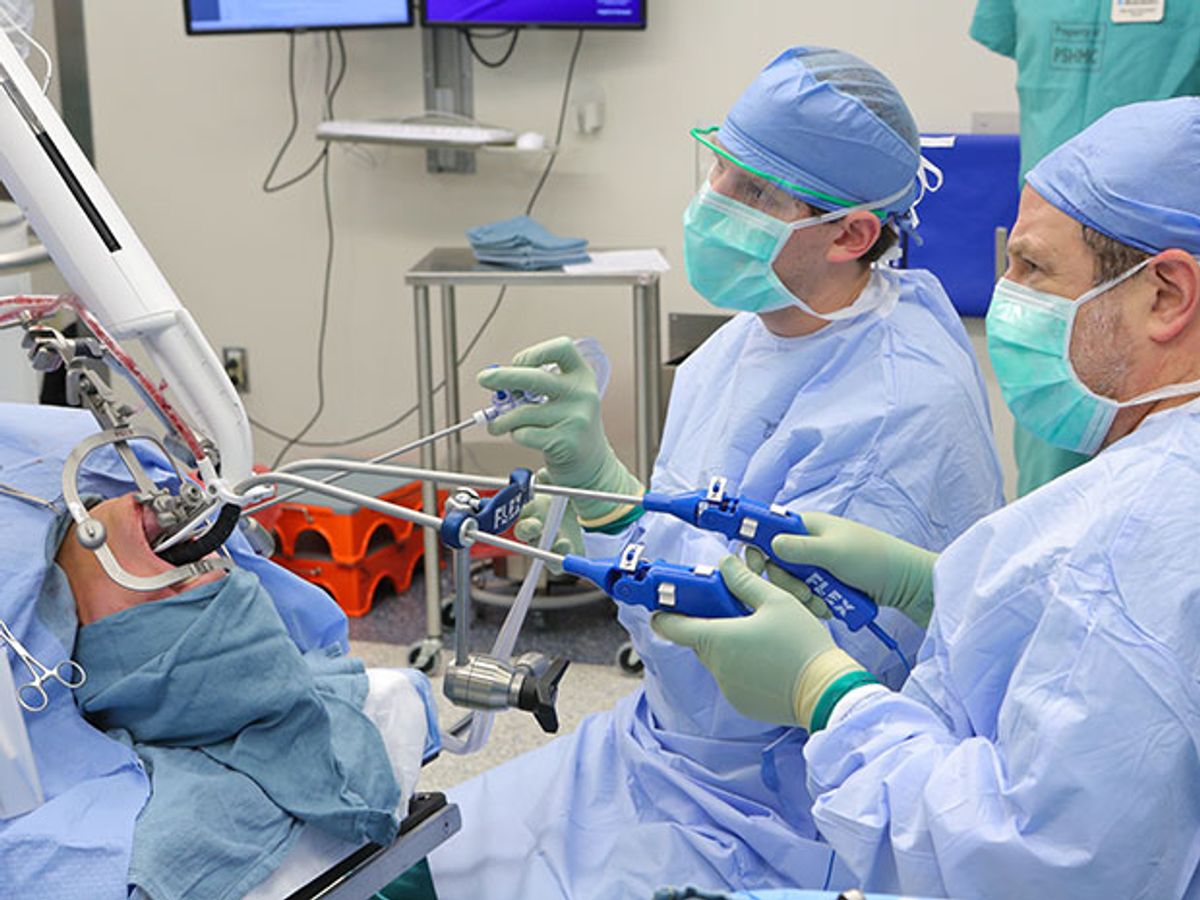
The Flex is, as its name implies, a flexible tube-like thing. The surgeon guides it into the patient’s mouth and steers it with a joystick; a camera at the Flex’s tip lets the surgeon see and navigate the twists and turns of the patient’s airway. Since it can reach otherwise inaccessible spots, surgeons like Goldenberg are using it for operations that would otherwise require them to crack the patient’s jaw or make an incision. Goldenberg says it makes many procedures cheaper, easier, faster, and less traumatic to his patients.
Once the Flex reaches the surgical target, it stiffens to provide a stable platform for instruments—which the surgeon inserts through two smaller tubes on the sides of the main conduit. The surgeon can swap in tools from a kit that includes scalpels, scissors, grippers, and a needle driver for suturing. (See the animation at this post’s end for a full tour of the tech.)
To move the Flex, the surgeon presses a switch on a controller. But Straface explains that the system also includes a foot pedal that controls the power to the overall system, turning the motor on or off. For the bot to move forward, the surgeon has to have a foot pressing down on the pedal. “It’s overkill,” says Straface. “This is an example of how the FDA drives the design.”
Only one autonomous feature was permitted in the Flex: Once the bot’s work is done, it can steer itself back up and out of the patient’s body. That independent movement is considered acceptable because it’s just reversing the path that the human surgeon plotted on the way in, Straface explains.
He hastens to say that everyone at Medrobotics is very glad that regulators obsess about patient safety. Sticking hard robots into people’s soft bodies is inherently dangerous, and no one wants a bot going rogue inside an airway or digestive tract.
And that safety imperative may point the way to a particular kind of R&D on robotic autonomy. If a smarter surgical tool can make a procedure less risky, the FDA may give it approval. For example, an inserted tool could have more sensing capabilities and could give the surgeon more feedback—for example, sounding an alarm or stopping short if it’s about to collide with tissue, says Straface. “It won’t be autonomy for the sake of taking the surgeon out of the picture,” he says. “That will not fly.”
Goldenberg, for one, says he hopes there will never be a fully automated surgical robot. “Not because I’m afraid of being replaced,” he says, “but because surgery is an art form that requires judgment and decision-making.” Besides the decisions about how to do a procedure, there are also larger life-and-death decisions, like recognizing when a disease has progressed so far that the surgery won’t be effective. “Surgery requires judgment, morals, and ethics that robots do not possess,” Goldenberg says.
The Medrobotics team isn’t trying to build an artificially intelligent surgical robot that understands moral reasoning. But Straface thinks robotic evolution toward autonomy will continue, even if it doesn’t result in the impressive humanoid robo-surgeon some enthusiasts envision. And it won’t be the first time that humans have settled for less, he says. “If you went back to the ‘60s and polled all the roboticists, they universally thought that we’d have humanoid robots doing housework by now,” he says. “Instead we got dishwashers and the Roomba.”
Eliza Strickland is a senior editor at IEEE Spectrum, where she covers AI, biomedical engineering, and other topics. She holds a master’s degree in journalism from Columbia University.