Researchers have made a smart contact lens and eyeglass combination that could be used to monitor diabetes and dispense drugs on-demand. The system includes cool-looking eyeglasses that wirelessly power and communicate with the circuit-lined, drug-releasing lens that a patient could wear for up to a month.
If it works, it could mean an end to the multiple painful finger pricks diabetics endure every day to monitor blood glucose levels. And it would be an easy, efficient way to treat the blindness-causing eye diseases that are common complications of diabetes.
The remote-controlled lens might also be used to treat other eye diseases and infections, says Sae Kwang Hahn, a professor of materials science and engineering at Pohang University of Science and Technology in Korea (POSTECH). Hahn and his graduate student Do Hee Keum presented their work on the lens system at the recent World Biomaterials Congress.
Diabetic retinopathy and glaucoma are the top two causes of vision loss and blindness in the world. Retinopathy refers to the damage that high sugar levels can wreak on the tiny blood vessels in the retina. Glaucoma, meanwhile, is optic nerve damage due to high pressure in the eye. Eye drops that lower eye pressure are a common treatment for glaucoma, and scientists are now investigating various peptide and chemical drugs in the form of eye drops for retinopathy, too.
Animal tests have shown that glucose concentration in tears is an effective proxy for blood sugar levels, Hahn says. The new lens-eyeglass system is a convenient way to constantly measure glucose levels in diabetics, alert the wearer to high levels, and provide therapy for diabetes-related eye disorders.
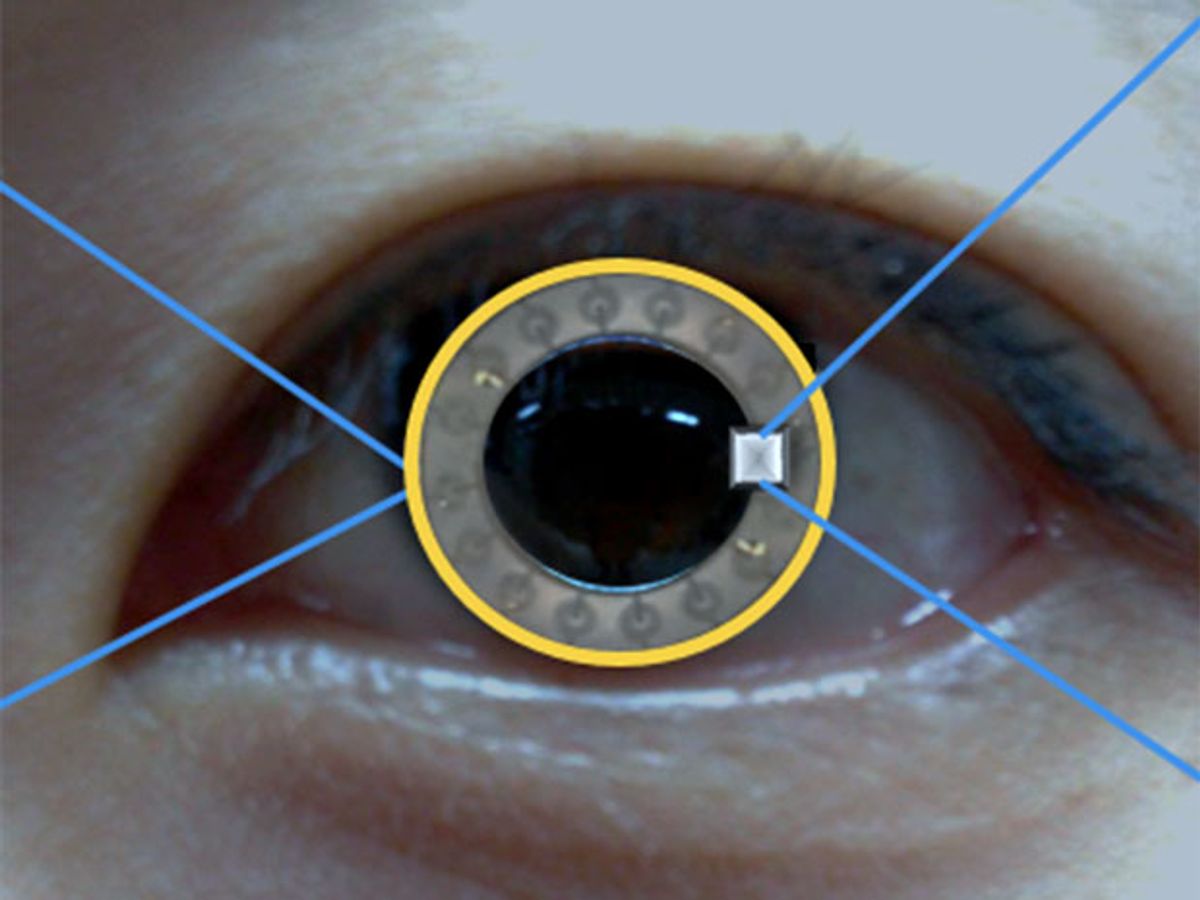
The lens is made of two soft silicone hydrogel layers that sandwich a ring-shaped circuit. The circuit has four components: an electrochemical glucose sensor, microcontroller chip, drug-delivery system, and an inductive coil to receive wireless power from the glasses. When tear glucose levels rise, the sensor’s current output increases and the chip relays this information wirelessly to the eyeglasses. An LED on the glasses lights up as an alarm in case of very high sugar levels.
The user can use voice commands to tell the eyeglasses to send a drug-releasing signal to the chip. In the future, a control circuit on the eyeglasses could make the process automatic, deciding on its own when drugs are needed. To release drugs, the chip zaps one of ten drug reservoirs, which are tiny chambers that the researchers carved into the hydrogel and covered with a thin gold electrode membrane. The voltage dissolves the membrane and releases the drug.
Tests of the sensor placed in an artificial tear solution showed that it worked accurately, with no drop in current, for three weeks when the researchers repeatedly spiked glucose levels. Since there are multiple drug doses on the lens, it could be used for up to a month, Hahn says.
Google and Novartis are working on a similar idea. Google received a patent in March 2015 for a diabetes-monitoring contact lens. While the patent mentions a reader device that would power and communicate with the contact lens, it does not specify details for such a device. Plus, says Hahn, “the unique feature of our smart contact lens is a flexible drug-delivery system.” He got a patent on the design with his colleagues at POSTECH and at the Massachusetts General Hospital at about the same time as Google.
Meanwhile, others are working on contact lenses that measure eye pressure, and Swiss company Sensimed already sells such a pressure-sensing lens in Europe. More recently researchers reported a wristband that measures glucose levels and injects drugs into the bloodstream via microneedles.
All of these concepts could be life-changing for diabetics, but only if any of them are reliable and affordable.
Prachi Patel is a freelance journalist based in Pittsburgh. She writes about energy, biotechnology, materials science, nanotechnology, and computing.