For people with diabetes, the need to prick fingertips with a lancet every few hours is now over. The advent of sensors for continuous glucose monitoring (CGM) means that patients can read their blood sugar levels in real-time, without the pain and hassles of repeated finger sticks. The latest CGM device, approved in September, doesn’t even require a finger stick for calibration, as other technologies do.
But all existing systems are still invasive, expensive and unsightly—involving a clearly visible sensor worn on the arm or abdomen with a tiny needle that enters the skin. And what the community really needs, says Daniel Finan, a research director at JDRF, the non-profit organization formerly known as the Juvenile Diabetes Research Foundation, is a glucose tester that’s cheap, accurate, non-invasive and inconspicuous.
Enter the new skin-like biosensor system reported today in the journal Science Advances.
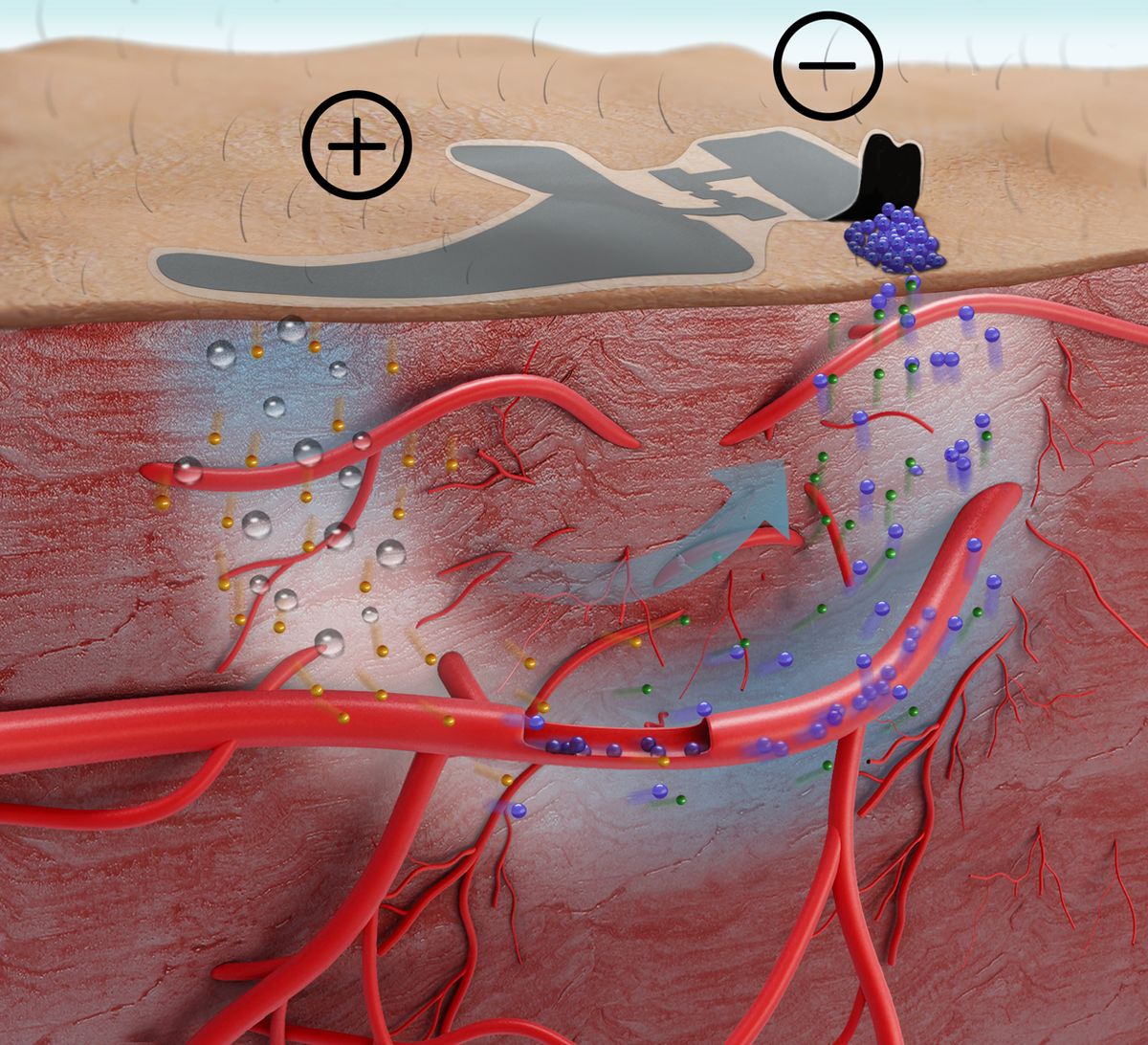
It involves first attaching a paper battery to the skin surface to create an electrochemical gradient in the tissue below. The wearer then applies hyaluronic acid—a common ingredient in skin-care products—to the battery’s anode, which pushes the positively charged molecule into the subcutaneous fluid. This changes the osmotic pressure encountered by the blood vessels that run through the skin, causing them to release more glucose that flows to the battery’s cathode at the skin surface.
After 20 minutes, the battery is then removed and the biosensor stuck on. It might look like just a tiny square of gold foil, but packed into the gossamer-thin film are five different layers that help convert the sugar molecules into electrical signals that can be read by standard laboratory equipment—or perhaps one day by a small and wearable circuit board.
The manufacturing of this 3-micrometer thick device was no small feat. “The whole fabrication process was a multidisciplinary task,” says Yihao Chen, a PhD student at Tsingua University’s Center for Flexible Electronic Technology and the study’s first author. “It consists of biochemistry, electrochemistry, medication, electrical design, semiconductor fabrication and fluid/solid mechanical transfer printing and analysis.”
But Chen and his colleagues, led by mechanical engineer Xue Feng, succeeded, and they then worked with a nearby hospital in Beijing to test the system on three people: two younger healthy subjects and a 62-year-old woman with type 2 diabetes.
As with all CGM devices that measure glucose indirectly through skin fluid, rather than in the blood, there was a time lag in the sensor’s ability to quantify glucose levels. But the system proved highly accurate, as gauged against finger sticks or blood drawn through an arm vein at multiple time points. And it did so without any signs of irritation, pain or inflammation at the skin surface—unlike some other non-invasive glucose monitoring systems that have been tried.
“We’re always driving toward discretion and really getting devices that adhere to your skin as a true patch would,” says Finan. So, “it might be that this is going to better solution than what’s currently out there.”
As yet, though, the new system is not capable of continuous monitoring. It can only measure glucose collected over the time the battery is on the skin. The same location on the body can be used over and over again, but a new battery and biosensor are needed for each and every reading.
That means “it’s not entirely seamless yet,” says Jacqueline Linnes, a bioengineer at Purdue University who is developing her own biosensor for reading glucose levels from someone’s breath. “But it’s a nice example of how you can get these kinds of skin-conformal devices to detect glucose.”
According to Chen, his team hopes to integrate the biosensor and voltage source to create something that’s suitable for CGM and could possibly be paired with an insulin pump to create a closed-loop “artificial pancreas” system. “We are working with a team from industry,” he says, “to further develop the system and make it more precise, compact and reliable.”
Elie Dolgin is a science writer specializing in biomedical research and drug discovery. After a PhD spent studying the population genetics of nematodes, he swapped worms for words—entering journalism as an editor at The Scientist, Nature Medicine, and STAT. Now a freelancer, Elie is a frequent contributor to New Scientist, Nature, IEEE Spectrum, and more.