Powered prosthetic legs work better when guided by electrical signals generated by the muscles, says a report published today in the Journal of the American Medical Association (JAMA). The findings suggest that bionic legs that rely on mechanical sensors to control movements would be greatly improved by the inclusion of electromyographic (EMG) data and the algorithms that interpret them.
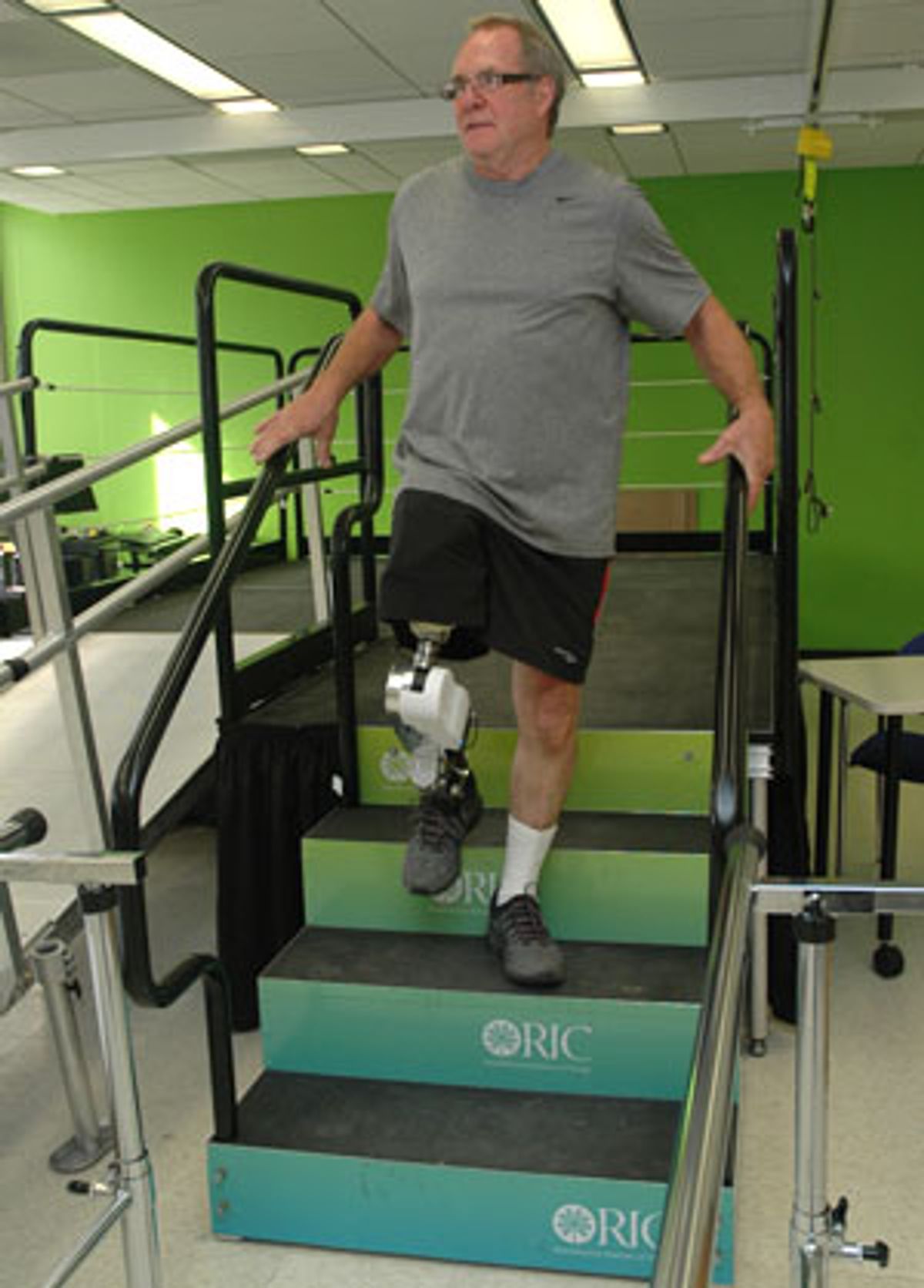
In the study, teams from the Rehabilitation Institute of Chicago and Northwestern University tried out their system on seven people with above-knee amputations. Each participant was outfitted with 9 EMG sensors on their thighs and hips that were connected to a computer. The participants wore a prototype knee-ankle prosthesis powered by 13 mechanical sensors that measured inertia, load, position, angle, acceleration, velocity and torque of the knee and ankle joints. The prosthesis was developed by Michael Goldfarb, a mechanical engineering professor at Vanderbilt University.
The participants were asked to traverse varying terrain—up ramps, stairs, and across level ground. The prostheses relying on the mechanical sensors alone made errors 14.1 percent of the time. But when the EMG data was incorporated, the prostheses made errors only 7.9 percent of the time—or about half as often.
“That’s a lot,” says Levi Hargrove, a research scientist at the Center for Bionic Medicine at the Rehabilitation Institute of Chicago, who led the study. The seven participants were not told when the EMG data was being used, but “every subject figured it out,” said Hargrove. “At the end of the experiment, we would ask: ‘Which of the two conditions did you prefer?’ And they chose the one that used the EMG signals every time.”
The advance is good news for people with above-knee amputations. Designing prostheses for these kinds of amputations is complex because they require precise coordination of knee and ankle movements. Particularly tricky is transitioning from one type of walking to another—like from walking on flat ground to climbing stairs.
There are only two powered leg prostheses on the market. One, which provides movement in just the knee joint, is made by an Icelandic company called Ossur. The other, called Biom, has a moving ankle; it was developed by Hugh Herr’s group at MIT. Prosthetics that combine powered knee and ankle movement are all still in the prototype stage.
A problem with these mechanical prototypes is that their designs don’t offer the flexibility necessary to accommodate different gaits. The user has to stop moving and make some kind of exaggerated body motion, or use a remote control to tell the leg what to do next—a problem that is frequently awkward and potentially dangerous.
Hargrove’s team aims to make walking smoother and safer for people with prosthetic legs. “We want them to be able to approach and walk up stairs the same way you and I would,” says Hargrove.
Arm prostheses are much more advanced than those for the legs. The “Luke Arm” developed by the DEKA Research and Development Corp, for example, harnesses EMG data from the amputee’s remaining arm muscles and interprets them to allow the prosthetic limb carry out multiple, simultaneous movements in the wrist and fingers that allow pinching or gripping. The device received FDA approval last year. Hargrove and his colleagues helped develop the system, and have since commercialized algorithms that can control the Luke Arm or any other arm prothesis that relies on EMG pattern recognition.
But systems for the leg—particularly for combined knee-ankle devices—have remained elusive. Why the difference? Arms have been a clinical focus for longer than legs. Plus, technological challenges—developing motors and actuators that are strong enough, light enough, and efficient enough to carry people throughout the day without having to recharge batteries—have been difficult to overcome. But that is changing. “All of these innovations are coming together to make these categories of devices available,” says Hargrove. “So now we need to learn to control them as best we can.”
Hargrove and his team, in a collaboration with Vanderbilt and the U.S. Army, are now testing the systems on 15 participants in home settings. “That’s the real test,” says Hargrove. “We’re trying to understand if this is useful for people in the real world.”
Emily Waltz is a features editor at Spectrum covering power and energy. Prior to joining the staff in January 2024, Emily spent 18 years as a freelance journalist covering biotechnology, primarily for the Nature research journals and Spectrum. Her work has also appeared in Scientific American, Discover, Outside, and the New York Times. Emily has a master's degree from Columbia University Graduate School of Journalism and an undergraduate degree from Vanderbilt University. With every word she writes, Emily strives to say something true and useful. She posts on Twitter/X @EmWaltz and her portfolio can be found on her website.