THE INSTITUTE While Mark Humayun was attending medical school in the 1980s at Duke University, in Durham, N.C., his grandmother began to lose her eyesight because of complications from diabetes. After deciding to research how he could use technology to help her retain her eyesight, he spent the next 20 years looking for a solution.
That journey ultimately led Humayun, an IEEE Fellow, to help invent the Argus II, a retinal prosthesis system approved in 2013 by the U.S. Food and Drug Administration. The first implantable device for people with retinal neurodegenerative diseases, it has helped more than 300 patients worldwide for whom there was no foreseeable cure.
Humayun, a professor of ophthalmology and biomedical engineering at the University of Southern California, in Los Angeles, built the Argus II with three other faculty members, after working on the original Argus. He also is director of the university’s Ginsburg Institute for Biomedical Therapeutics.

For his work, Humayun is the recipient of this year’s IEEE Medal for Innovations in Healthcare Technology. The award, which is sponsored by the IEEE Engineering in Medicine and Biology Society, is scheduled to be presented at the annual IEEE Honors Ceremony, during the IEEE Vision, Innovation, and Challenges Summit, to be held on 15 May in Vancouver.
Humayun received his medical degree in 1989 from Duke and a Ph.D. in biomedical engineering in 1994 from the University of North Carolina at Chapel Hill.
He is the only ophthalmologist ever to have been elected as a member of both the National Academy of Medicine and the National Academy of Engineering.
The IEEE Medal for Innovations in Healthcare Technology is not the first honor Humayun has received for the Argus II. In 2016 he received a U.S. National Medal of Technology and Innovation, presented by President Barack Obama.
“It’s very gratifying when peers acknowledge you,” Humayun says. “Certainly, it rises to a different level when the president of the United States gives you a national award. It was one of the highlights of my career.”
The path to developing the Argus II wasn’t easy.
“No one believed in the project at first,” Humayun says. “It took over a decade to build the team to what it is now and to increase the faith physicians and engineers have in the technology.”
FINDING INSPIRATION
Two research projects that experimented with electrodes inspired the technology behind the Argus II.
While investigating how technology could help his grandmother’s vision, Humayun discovered research that was being conducted into the causes of epileptic seizures. Physicians were stimulating the patient’s occipital lobe—the brain’s vision center—with electrodes, hoping to determine whether that part of the brain caused seizures.
“When the surgeon touched the occipital lobe, the patient would see a spot of light even though there was no light,” Humayun says. “That discovery made me think: Could electrical stimulation be used to restore eyesight?”
During the same period, another innovation was being developed: cochlear implants, surgically implanted electronic devices that provide a sense of sound to people who are deaf or severely hard of hearing. The implants use electrodes to stimulate the auditory nerve.
The Argus II is not able to restore full vision, but it can offer a person some functional sight: the ability to see boundaries and outlines of objects and people—which can help them navigate their environment.
HELPING PATIENTS SEE
The Argus II is made up of wearable components and an implant. The device, which bypasses the light-sensing cells in the eye, can be used by patients age 25 and older who don’t have damaged optic nerves. If an optic nerve is damaged, as occurs with glaucoma and other conditions, the implant can’t stimulate it.
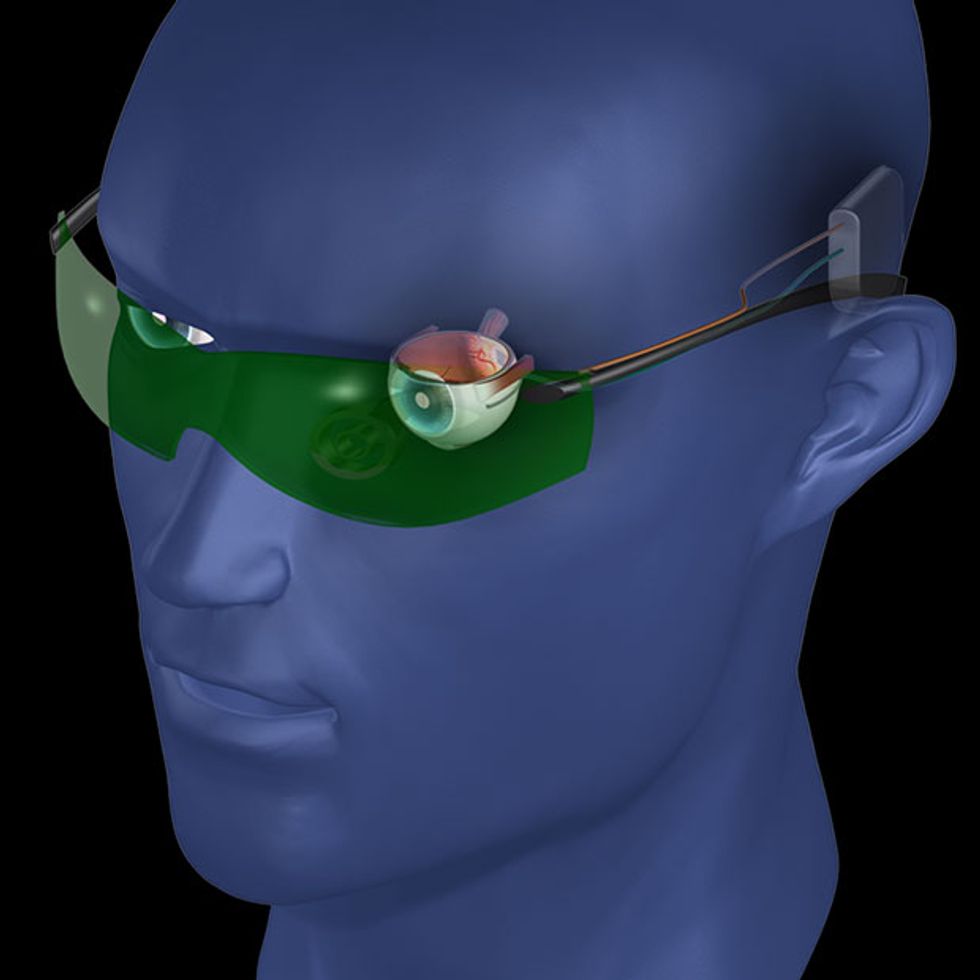
The implant includes a receiving coil; an antenna, which is placed under the muscles around the eye; and a 60-electrode array. The array is surgically placed in the back of the patient’s eye, connecting it to the retina’s remaining neurons. It sends information to the brain’s visual center via the optic nerve.
To create information the implant can use, the patient wears eyeglasses containing a miniature camera, which captures video of the scene in front of the wearer. That information is then sent wirelessly to a processor, which is about the size of a cellphone and can be worn on a belt or carried in a pocket. The processor converts the video into instructions that are sent wirelessly to the implant. The implant’s electrodes then stimulate the retina, allowing the patient to decipher the image the camera captured as flashes of light.
“The electrode array electrically stimulates and jump-starts the otherwise blind eye,” Humayun says.
Each patient meets with an occupational therapist or low-vision therapist to relearn how to function with sight. Patients also are required to return periodically to their ophthalmologist to get the software and the system’s electronics adjusted to meet their changing needs.
OVERCOMING CHALLENGES
When Humayun and his team first began the Argus project, they had to resolve several issues with hardware and software. How, they wondered, do you make a device that doesn’t deteriorate in the eye? And what kind of electrical pulses could be viewed as an image?
After working on the device for more than 15 years, the team began clinical trials in 2007, testing the technology on patients for 30 minutes without implanting it. The first patient was able to see for the first time in the very first test session after having been blind for 50 years.
“Witnessing the first patient see a spot of light for the first time was a defining moment for me and the project,” Humayun says.
After news spread that the test was successful, more engineers, physicians, and scientists sought to join Humayun’s team, which now includes more than 200 people.
Humayun says his IEEE membership helped him raise awareness of his work. “The organization helped me connect with engineers from many different fields, such as biomedical, electrical, industrial, and mechanical.”
Two IEEE Fellows who joined Humayun’s team were instrumental in its success: Gianluca Lazzi and James Weiland. Lazzi is an engineering professor at USC who specializes in antennas and wireless communication. Weiland is a professor of bioengineering and ophthalmology at the University of Michigan in Ann Arbor.
“Mark has accomplished extraordinary things at the intersection of engineering and medicine in his career,” Lazzi says. “His pioneering contributions to the field of artificial sight are so unique, fundamental, and visionary that they have created a paradigm shift in entire fields. I am incredibly excited about what lies ahead.”
Joanna Goodrich is the associate editor of The Institute, covering the work and accomplishments of IEEE members and IEEE and technology-related events. She has a master's degree in health communications from Rutgers University, in New Brunswick, N.J.



