In the 1960s, a pacemaker was the size of a microwave and a dialysis machine was the size of a refrigerator. Today, a pacemaker is the size of a vitamin and a dialysis machine is, well, the size of a refrigerator. They do have nice LED displays though.
“Kidney disease is underserved,” says Shuvo Roy, a bioengineer at the University of California, San Francisco. Although failed kidneys kill more people each year than breast or prostate cancer, “the field has not seen much innovation in the last 50 years,” says Roy.
The U.S. Department of Health and Human Services and the American Society of Nephrology want to change that. The organizations have teamed up to bring money and attention to the disease with the KidneyX: Redesign Dialysis competition. Started in 2018, the competition challenges innovators in any field to propose tools and technologies that could enable the design of new artificial kidney devices.
The average wait time for a kidney transplant is 3.6 years, according to the National Kidney Foundation, and 13 people die each day waiting for one. As they wait, patients receive four hours of dialysis three times a week. The treatment sustains life but does not restore health.
The 15 winning teams for Phase 1 were announced on 29 April at the KidneyX Summit in Washington, D.C. Participants were asked to submit an abstract about a proposed solution, and each winner will be awarded $75,000 to develop their design.
“The winning proposals address a broad range of potential improvements to dialysis and highlight the fact that there is more work to be done to change the status quo. Millions of patients are waiting,” said John Sedor, chair of the KidneyX Steering Committee, in a press release.
Here’s a sampling of the winners (see the full list here):
A device added to dialysis catheters to better prevent infection and blood clots.
A sensor-enhanced needle guide so patients can safely receive dialysis at home.
A wearable device to identify blood clots in real-time.
A blood-filtration unit using silicon filters that patients could operate at home.
That last proposal comes from The Kidney Project, led by Roy at UCSF and William Fissell at Vanderbilt University, which has been working for the last decade to create a fully-implantable artificial kidney. “An implanted device would allow a patient to move freely and provide continuous treatment,” he says.
Small squares of a silicon membrane, shown here on a slide, filter blood for The Kidney Project's bioartificial kidney design and iHemo device.Photo: Steve Babuljak/UCSF
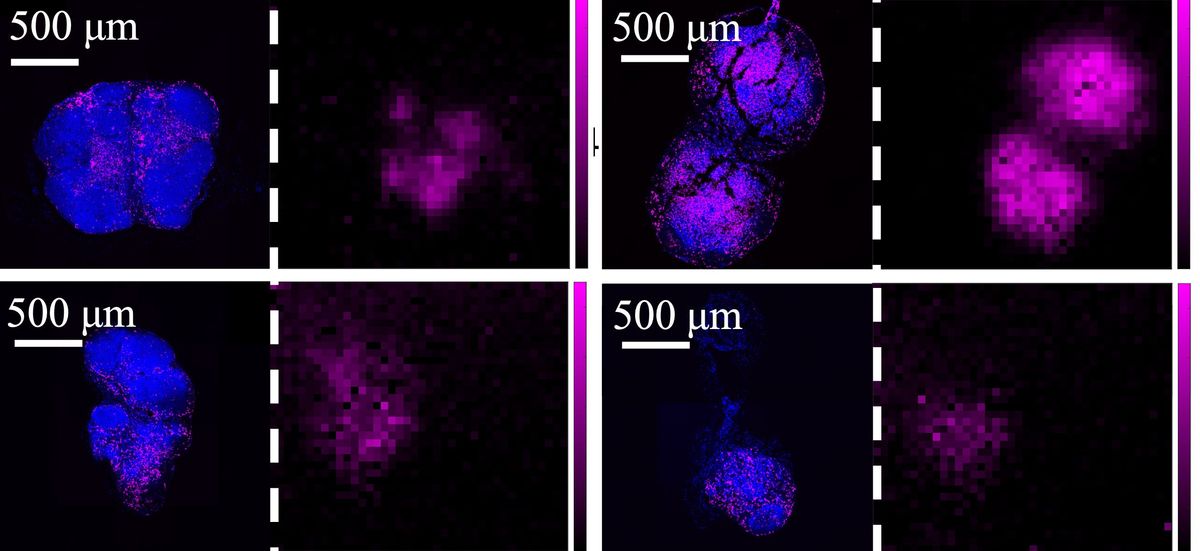
Their current implantable design has two main components: a mechanical filtration unit that performs the cleansing functions of a kidney with silicon membrane filters; and a bioreactor unit lined with kidney cells to take care of the other key functions of a kidney, such as salt and water reabsorption, regulating blood pressure, and producing vitamin D.
Such a device could implant in the abdomen where a transplant kidney would be placed, serving as a “universal donor kidney,” says Roy. The team is now preparing to begin a human trial with the filtering unit. The kidney cell unit is being optimized and expected to soon move into animal testing.
For the KidneyX competition, Roy’s team used the same implantable blood filtration unit but connected it to an external dialysis pump system, called iHemo, that allows for self-care by patients at home. This hybrid device is a stepping stone, says Roy, as the true grail remains a fully implantable device.
Phase II of the competition is now open. This time, participants are challenged to build and test a prototype of their solution. Next year, three winners will walk away with $500,000 each. Submissions are due in January 2020, so it’s time to start building.
Megan is an award-winning freelance journalist based in Boston, Massachusetts, specializing in the life sciences and biotechnology. She was previously a health columnist for the Boston Globe and has contributed to Newsweek, Scientific American, and Nature, among others. She is the co-author of a college biology textbook, “Biology Now,” published by W.W. Norton. Megan received an M.S. from the Graduate Program in Science Writing at the Massachusetts Institute of Technology, a B.A. at Boston College, and worked as an educator at the Museum of Science, Boston.