Delivering drug-loaded nanoparticles to tumors is a brilliant way to kill cancer cells and reduce the drugs' side effects. But the nanoparticles can sometimes also kill healthy cells. Scientists at Rice University are now working on what they say is a more selective and effective technique that will deliver chemotherapy drugs right inside cancer cells without harming normals cells.
The method relies on using lasers to creating tiny bubbles around clumps of gold nanoparticles inside cancer cells. The nanoparticles don't carry drugs. Instead, as the bubbles burst, they temporarily rip open small pores in the cell membranes so that drugs present outside the cells can get in.
Rice's Dmitri Lapotko, a physicist and biochemist, said in a press release: "We are delivering cancer drugs or other genetic cargo at the single-cell level. By avoiding healthy cells and delivering the drugs directly inside cancer cells, we can simultaneously increase drug efficacy while lowering the dosage."
Specifically, the researchers have found that delivering chemotherapy drugs with nanobubbles was up to 30 times more effective at killing drug-resistant cancer cells than traditional chemotherapy, and required less than a tenth of the drug dose. So far, the team has tested the method on head and neck cancer cell cultures. They’ve published their results in three separate papers that have recently appeared in the journals Biomaterials, Applied Materials, and PLoS One.
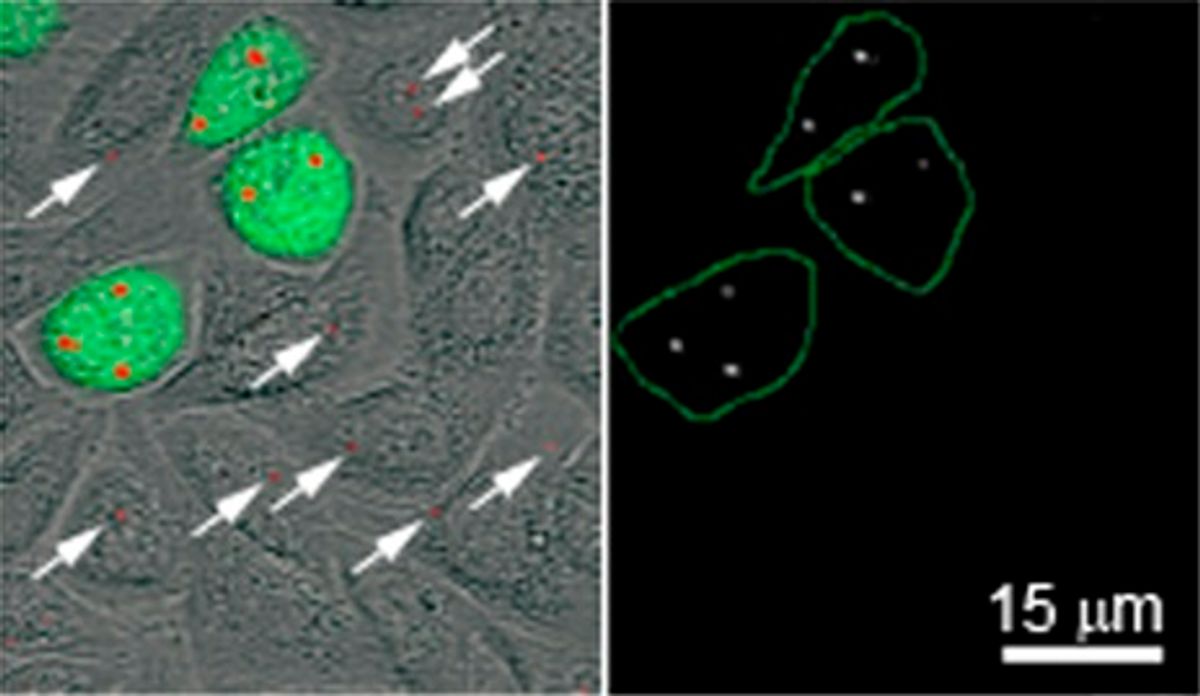
To make the bubbles, the researchers first have to get the nanoparticles inside cancer cells. They do this by tagging the particles with antibodies that almost exclusively attach to the surface of cancer cells, which then ingest the particles. The nanoparticles form clusters just below the cells’ protective outer membranes.
Then the researchers zap the cells with short near-infrared laser pulses. The laser’s wavelength is tuned to that of plasmons, or electron oscillations, on the surfaces of the gold nanoparticles. The particles convert the light into heat, which evaporates some of the surrounding medium, creating small vapor bubbles that expand and burst within nanoseconds.
In cultures containing a mix of normal cells and cancer cells, the researchers showed that the nanobubble technique only killed cancer cells. Healthy cells are spared because they take up far fewer nanoparticles than the targeted cancer cells. The laser energy isn’t enough for the smaller nanoparticle clusters to form bubbles and rupture the membranes of healthy cells.
Animal tests are next.
Image: PLoS ONE
Prachi Patel is a freelance journalist based in Pittsburgh. She writes about energy, biotechnology, materials science, nanotechnology, and computing.