The symptoms of post-traumatic stress disorder and traumatic brain injury overlap in a dizzying blur of similarity: depression, difficulty concentrating, anxiety, fatigue, loss of interest, and more.
Mild traumatic brain injury (mTBI)—the result of the head being hit or violently shaken—and PTSD plague returning veterans and affect civilians: Each year, an estimated 8 million adults have PTSD and 1.3 million Americans sustain a mild brain injury.
Currently, there is no screening tool or instrument to reliably diagnose either condition. Instead, one’s best chance for an accurate diagnosis is an interview with a skilled physician. Due to the subjective nature of that process, many cases of each condition go undetected or misdiagnosed.
Now, a team at Cambridge, Mass.-based Draper, a not-for-profit research and development company, Harvard Medical School, and Brigham and Women’s Hospital is developing a non-invasive test to provide a straightforward diagnosis for either condition (or both). “It’s essentially a non-invasive biopsy looking at the chemical constituents of the brain, and trying to use that to make a diagnosis,” says John Irvine, Draper’s chief data scientist.
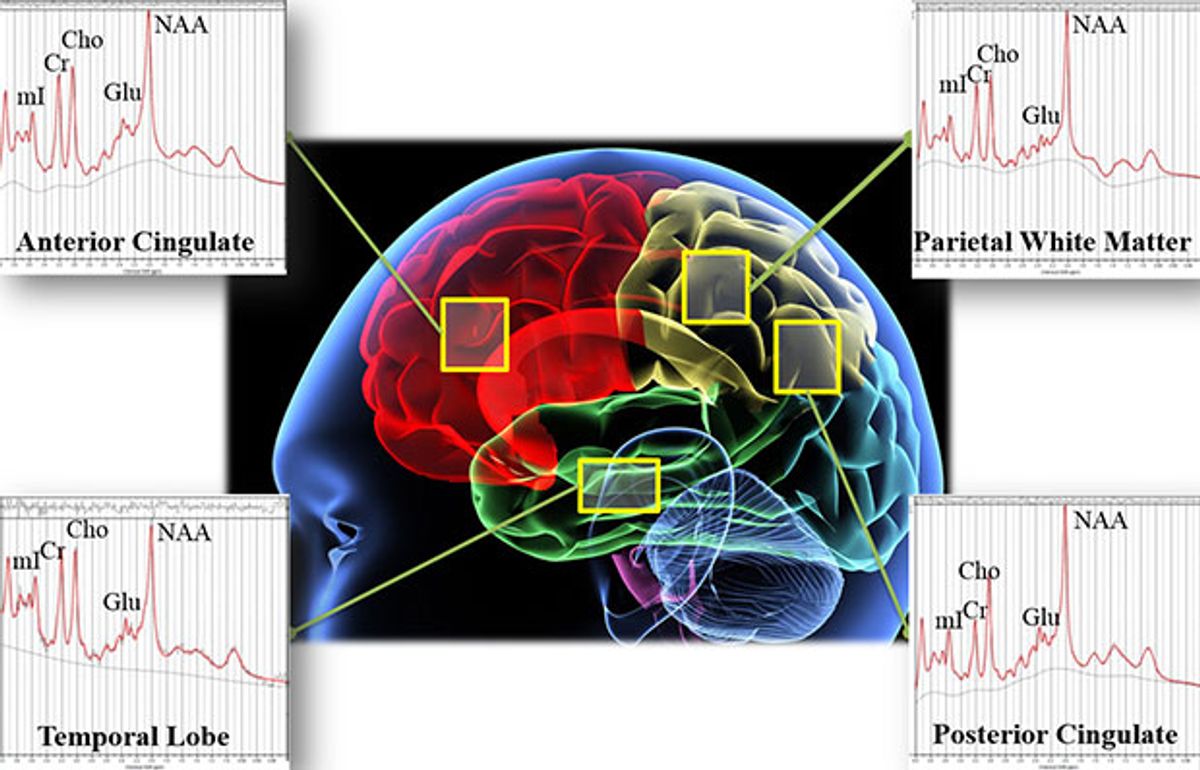
At the Center for Clinical Spectroscopy at Brigham and Women’s, Alexander Lin oversees the brain scans of veterans who have experienced a trauma, as well as healthy veterans and civilians as controls. Each participant lies down in a magnetic resonance imaging (MRI) machine. A typical MRI scan uses powerful magnetic fields to produce spatial images of the brain or other organs. Lin instead applies a different protocol, called magnetic resonance spectroscopy (MRS), to use the magnetic fields to detect levels of molecules in the brain called metabolites. His technicians scan four regions of each participant’s head, sections of approximately five cubic centimeters each, to capture a slew of raw data on the chemical composition of the brain.
Next, Irvine and his team apply a series of algorithms to clean and process that data, which is often noisy with weak chemical signals. The most abundant chemical in the brain is water, so the first step is to remove that signal from the data. After additional data processing, the team fits a set of wavelets (mathematical functions used to process signal information) to the processed MRS signals. These wavelets allow the team to identify unique metabolite peaks that may have been hidden in the original data heap.
In an initial test of the “virtual biopsy” in 18 patients, the team identified two potential biomarkers: Patients with mTBI had lower levels of the metabolites N-acetyl aspartate and creatine than PTSD patients. Irvine emphasizes that the results are preliminary.
“I’m reluctant to put too much credence into what we discovered from just a handful of patients,” says Irvine. “We’re excited about getting more data and seeing if these relationships hold up.”
To date, the team has scanned 75 individuals and plans to expand the study to several hundred over the next year in collaboration with additional hospitals. Irvine suspects that it will be more than just one or two metabolites in the brain that distinguish each condition, but a suite of metabolites that make up a chemical signature associated with each condition. If the researchers can discover and validate that signature, returning veterans could get the brain scan as part of routine care, hopefully for the same price as a traditional MRI scan.
The combination of MRS and the data analysis tools could also be useful in other brain conditions involving changing levels of metabolites in the brain. Draper has a second project using the technique to study chronic traumatic encephalopathy, the progressive degenerative brain disease affecting football players and other athletes who experience repetitive brain trauma.
“It’s a widely applicable tool,” says Irvine. “As we have more experience with it and collect more data, we’re going to find other medical conditions where it’s going to be useful.”
The work is funded by the Pentagon’s Congressionally Directed Medical Research Programs office.
Megan is an award-winning freelance journalist based in Boston, Massachusetts, specializing in the life sciences and biotechnology. She was previously a health columnist for the Boston Globe and has contributed to Newsweek, Scientific American, and Nature, among others. She is the co-author of a college biology textbook, “Biology Now,” published by W.W. Norton. Megan received an M.S. from the Graduate Program in Science Writing at the Massachusetts Institute of Technology, a B.A. at Boston College, and worked as an educator at the Museum of Science, Boston.