Jessica Morris was on a hiking trail in upstate New York last January when she suddenly uttered a line of gibberish and fell to the ground, her body shaking in a full seizure. A few hours later in a hospital she learned that she had an aggressive brain tumor, and several days after that she was on the operating table having brain surgery. Since then, she’s been fighting for her life.
She’s grateful to have a radical new weapon in her arsenal, one that only became available to patients like her in 2015. She wears electrodes on her head all day and night to send an electric field through her brain, trying to prevent any leftover tumor cells from multiplying. She’s been wearing this gear for about six months so far. “I think it’s brilliant,” Morris says. “I’m proud to wear it.”
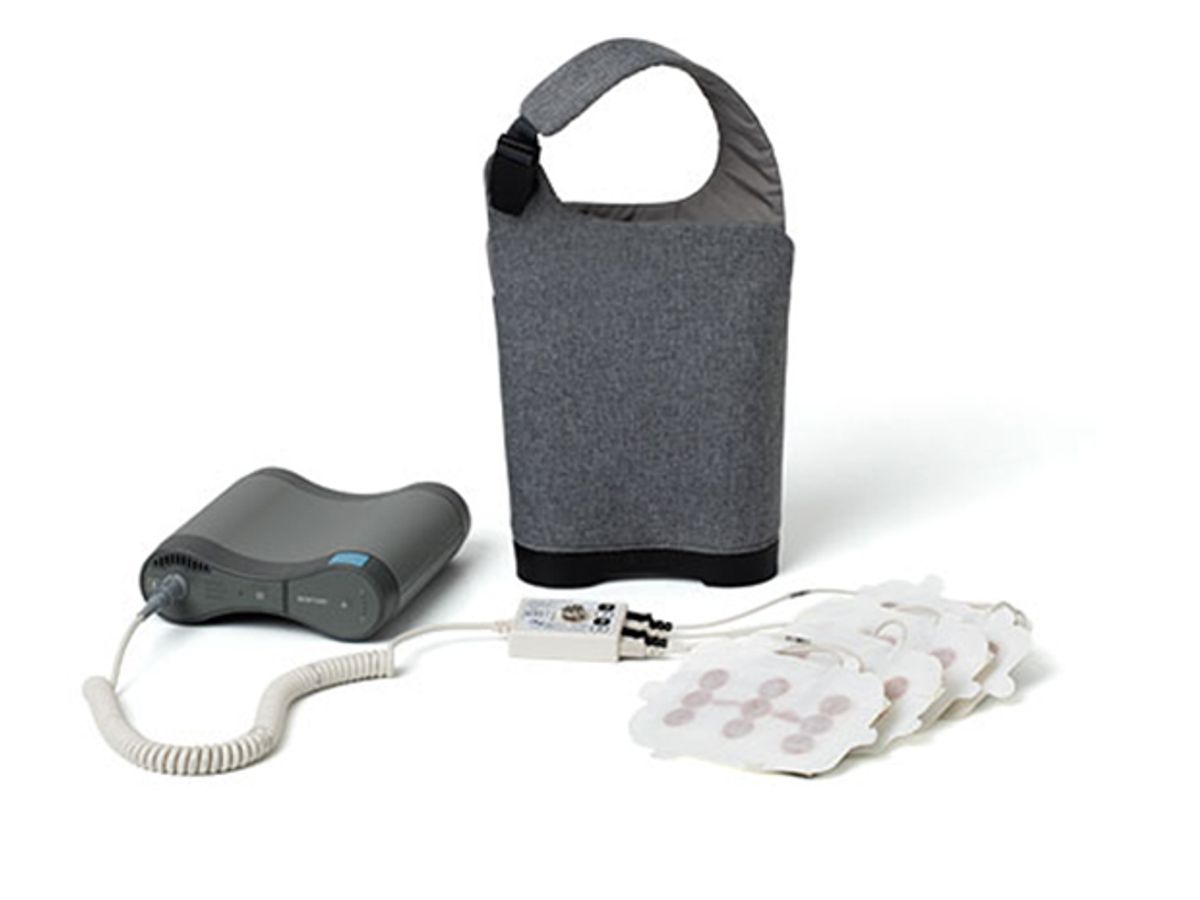
The Optune device, invented by a company called Novocure, can’t exactly be called convenient or unobtrusive. Morris goes about her business with a shaved head plastered with electrodes, which are connected by wires to a bulky generator she carries in a shoulder bag. Every few days her husband helps her switch out the adhesive patches that hold the electrodes, which requires reshaving her head, making sure the skin of her scalp is healthy, and applying the new patches.
Morris isn’t complaining about the effort. “If you have a condition which has no cure, it’s a great motivator,” she says dryly.
Optune wasn’t the obvious choice for Morris’s fight against the tumor she calls “the evil f**ker.” She has glioblastoma, the most common and malignant form of brain cancer. Doctors typically combat glioblastoma with the triad of surgery, radiation, and chemotherapy.
Optune’s tumor-treating fields (TTFs) offer an entirely new type of treatment. Unlike chemo, this electrical treatment doesn’t cause collateral damage in other parts of the body. Yet many oncologists remain skeptical of the technology. “The adoption rate has not been stellar to date,” admits Eilon Kirson, Novocure’s chief science officer.
Last Friday’s announcement could change things. At a neuro-oncology conference, researchers reported the results of Optune’s big clinical trial, which looked at survival rates among 695 patients with glioblastoma. Two years after beginning treatment, 43 percent of patients who used Optune were still alive, compared to 30 percent of patients on the standard treatment regimen. Four years out, the survival rates were 17 percent for Optune patients and 10 percent for the others. “To patients, that’s a big difference,” Kirson says. “That’s worth fighting for.”
Kirson says this long-term data should convince neuro-oncologists, and he hopes that other cancer specialists are paying attention too. “The therapy really revolutionizes glioblastoma care,” Kirson says. “And more than that: It introduces a new modality that will hopefully transform cancer care.” The company has ongoing trials for pancreatic, ovarian, and lung cancer.
Brain cancer was a daunting disease to tackle first, says Novocure executive chairman William Doyle, because brain tumors are notoriously tough to fight. The last advance in treatment came about 15 years ago when doctors introduced a new chemo drug, temozolomide. “Since then, every attempt to make an improvement in these patients’ survival rates has failed,” Doyle says. Until Nococure’s attempt, he means.
At a recent conference on bioelectronic medicine, Doyle recounted his company’s decades-long struggle to gain regulatory approval and medical acceptance of the Optune technology. “If this came in a bottle, 100 percent of glioblastoma patients would be taking it,” he says.
In 2011, Novocure’s technology was approved in the United States for patients with recurrent glioblastoma—patients who were out of options. In 2015, regulators approved it for newly diagnosed glioblastoma patients as well. It’s also available now in Europe and Japan.
Novocure’s system uses electrodes stuck to the scalp to create a low-intensity AC electric field in the brain, which interfere with cancer cells as they try to divide and spread. The tumor-treating field has its impact when a dividing cell reaches its hourglass shape, a geometry that concentrates the TTF at the pinch point.
It’s long been known that molecules inside the cell are polarized and respond to electric fields. The TTF pulls those polarized molecules inside the cell into the wrong positions, messing up the precise sorting procedures of cell division. Or, as Doyle puts it, “all hell breaks loose inside the cell.” The cells don’t divide and may go into a state of programmed cell death.
So why do the TTFs hit tumor cells hard, while leaving normal cells unharmed? Doyle says the secret lies in the frequency of the electric field. Each different cell type has a membrane with specific filtering properties, allowing only certain frequencies to penetrate and enter the cell. (You can think of the cellular membrane as a capacitor, Doyle says; at the right frequency, the field can go through it with very little impedance.) Optune uses a frequency of 200 kHz, which gets inside glioblastoma cells but doesn’t penetrate neurons and other normal brain cells.
It doesn’t hurt that there’s very little cell division going on in the brain. In other parts of the body, normal healthy cells also divide frequently. So to gain approval as a treatment for other types of cancer, Novocure will have to carefully prove that its targeting trick works. If the company can do that, Optune may be tremendously useful. Because the treatment relies on a physical rather than a chemical mechanism, it could be broadly applicable regardless of cancer subtypes and genetics.
It’s too early to say whether the company really has discovered the next big thing in cancer treatment. Some oncologists are much more excited about up-and-coming immunotherapy treatments, which cause the body’s immune system to attack the tumor cells.
Neuro-oncologist Wolfgang Wick wrote about the field’s skepticism regarding TTFs in the journal Neuro-Oncology in March, basing his remarks on Novocure’s preliminary results from its clinical trial. He noted that the trial couldn’t be sham-controlled, which is considered the gold standard for medical trials, since it wasn’t appropriate for some patients to be burdened with wearable gear yet only receive sham treatment.
Wick says the new long-term results from the trial don’t change his outlook. He also draws a contrast with the chemo drug temozolomide, which provides clear benefit to a subset of patients who have a particular biomarker. Doctors don’t know which patients will respond best to the tumor-treating fields, he tells IEEE Spectrum, and that makes Optune a less appealing treatment option. “If I listen to my patients, this is one thing missing with the TTF and this has not changed,” Wick says.
And then there’s the comfort factor. Many doctors and patients would probably prefer a treatment that doesn’t require 24-7 wearable hardware.
Novocure just upgraded Optune, reducing the size and weight of the external field generator and its battery pack. The first-generation generator weighed about 3 kg (6 pounds) and came in a backpack, while the new version weighs 1.2 kg (2.7 pounds) and comes in a shoulder bag. The user needs to change the batteries every few hours, or plug in to a wall socket.
Novocure recommends that patients keep their systems turned on for 18 hours each day, but Jessica Morris says she keeps hers running almost continuously. She mostly disconnects to take a shower, which requires unplugging the wires from the generator and coiling them under a special shower cap.
Morris isn’t sure how long she’ll be wearing Optune. Her doctor originally told her nine months but recently revised that estimate, saying she might want to keep it on for two years. That change in plans reflects her promising medical outlook: Her MRI scans haven’t shown any new brain tumor growth, and Morris wants to keep it that way. “If I’m still doing well, why would I take it off?” she says.
Morris says it can be irritating to be tethered to a piece of electronics. “I do feel a bit like a dog,” she says. “I have a leash.” But when she gets annoyed, she reminds herself that she’s pioneering a technology that is pushing the limits of the possible. “This is like the driverless car, it’s like going to Mars successfully,” she says. “As long as I focus on that, the cumbersome nature of it falls away.”
Eliza Strickland is a senior editor at IEEE Spectrum, where she covers AI, biomedical engineering, and other topics. She holds a master’s degree in journalism from Columbia University.