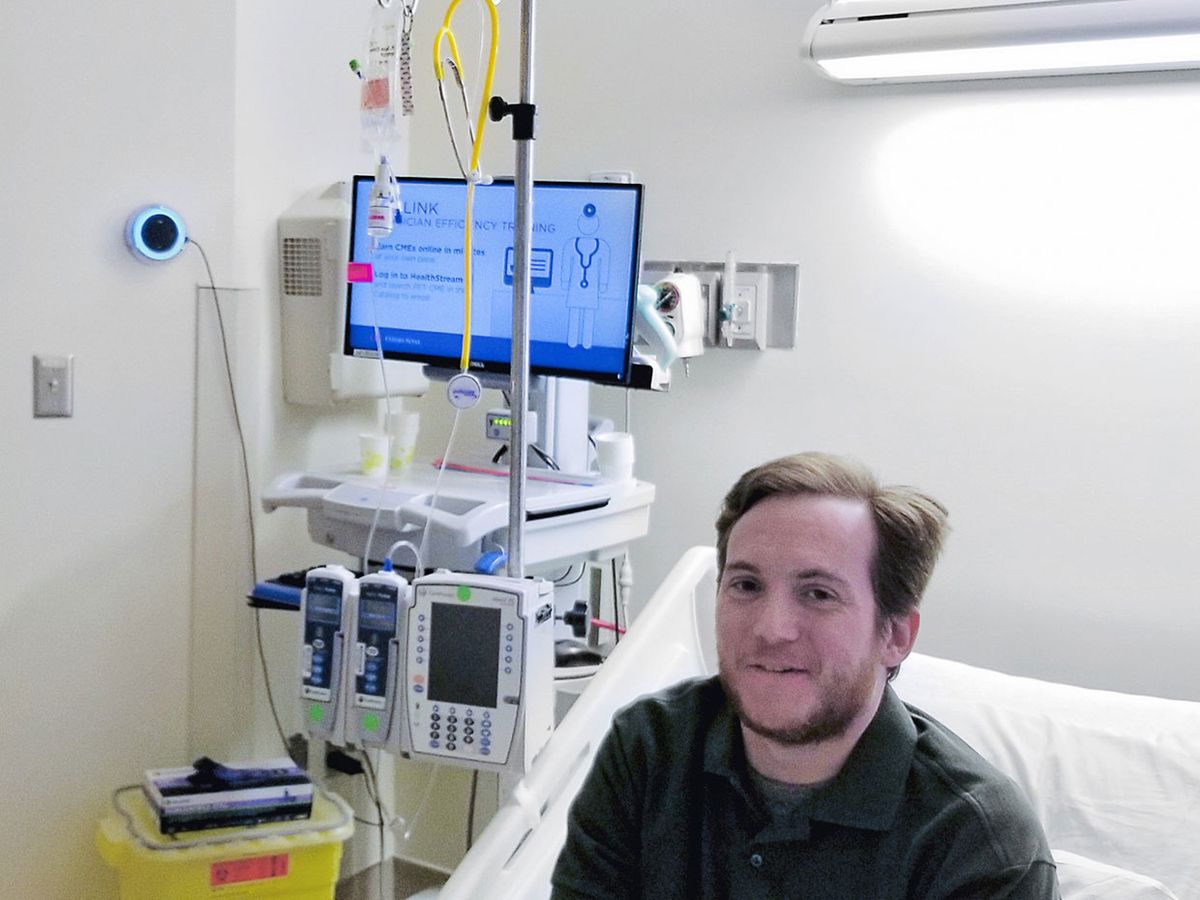
The 90-year-old man wheeled into the hospital room was agitated. A nurse, welcoming the patient and his wife, asked if either of them were familiar with Alexa. An Amazon Echo Dot mounted on the wall lit up in blue at the sound of its name. The man’s wife immediately asked Alexa to play classical music, and a melody filled the room. The patient calmed.
This scene occurred recently at Cedars-Sinai hospital, in Los Angeles, in one of the facility’s newly anointed “smart” hospital rooms, powered by an Alexa-based technology.
“If there’s nothing else Alexa can do but distract our patients from pain, anxiety, and loneliness in the room, that’s a win,” says Peachy Hain, executive director of medical and surgical services at the hospital who has overseen implementation of the technology.
As it turns out, Alexa can do a lot more than that. Early, anecdotal results from a pilot program at Cedars-Sinai show that an Alexa-powered platform called Aiva provides entertainment, connects patients with hospital staff and the outside world, and improves workflow for nurses.
The program began in February 2018 in just six hospital rooms to see if the amenity would be welcomed by patients and caregivers, says Hain. A year later, the program has expanded into 102 rooms across 4 units at the hospital.
Aiva, a voice assistant technology designed for healthcare, received early investment from Cedars-Sinai as part of the hospital’s accelerator program, says Aiva founder and CEO Sumeet Bhatia. While the pilot program at Cedars-Sinai relies on Amazon Echo devices, the company’s software is device-agnostic, says Bhatia: It can be used with Google Home devices and will extend to other third party products in the future. “We think of ourselves as the voice-operating system for healthcare,” he says.
In each room of the pilot program, an Amazon Echo Dot attached to the wall communicates with Aiva’s software, which transmits and tracks requests to devices in the room, such as the television, as well as to healthcare providers. When a patient asks for pain medication, for example, Aiva sends a text to the appropriate nurse. If the request isn’t fulfilled, the notification goes up the chain to another caregiver. Plus, Alexa responds to a patient by telling him or her that their request has been transmitted, providing comforting feedback that isn’t supplied by a traditional call button.
For now, Aiva will not replace call buttons, says Hain. For example, the system doesn’t work for all patients: Those with breathing tubes or patients who are in significant pain cannot operate the voice-activated system. And it currently only understands English, while the hospital serves a large Hispanic population that includes many non-English speakers.
Patients have been putting the system to use for music, turning on the TV, changing channels, and checking the weather and sports scores. Those activities are valuable, emphasizes Hain, because they give patients a connection to the outside world, helping them to feel less lonely. Younger patients naturally take to the technology faster, she adds, as they tend to be more familiar with it.
In a recent press release, abdominal surgery patient Adrienne Edwards described her enthusiasm for the technology: “It rocks,” Edwards said. “I was lonely in the hospital and I said, ‘Alexa, would you be my friend?’ The device responded, ‘Of course we could be friends. You seem very nice.’”
So far, nurses are also responding positively to the technology, says Hain. The hope is that by routing requests to the appropriate person—such as medication requests to a registered nurse and bathroom requests to an aide—it will free up registered nurses for actual nursing, rather than helping patients with the all-too-common request of finding the right television station, for example.
Currently, hospital staff are working hard to remind patients about the technology: After an initial introduction to Aiva upon admission, volunteers visit the rooms each day to remind patients that the Echo Dot is there and describe how the device can be used. Signs on the walls offer additional reminders that Alexa is available. “So far, we’ve found that you need to keep reminding people of something new—even the staff,” says Hain.
Moving forward, there are more tasks the staff and patients would like the technology to take over, especially turning on and off lights, says Hain. Working with Aiva, they hope to soon add the ability to route requests to more places in the hospital, such as food requests to the kitchen, transportation requests to wheelchair services, and even requests for a furry companion to the dog therapy team.
By the end of May, Hain hopes to have enough data for the hospital administration to make a decision about expanding or cutting back on the program. She’s optimistic: “Healthcare organizations need to keep up with technology, and we need to use technology to deliver our services to patients,” says Hain. “We’re very excited about this.”
Cedars-Sinai is no newcomer to applying tech innovations in clinical settings: The hospital boasts an iPad project that allows patients to check medical records and lab results from their bedside, and researchers at the hospital are testing the use of virtual reality headsets to reduce pain.
Megan is an award-winning freelance journalist based in Boston, Massachusetts, specializing in the life sciences and biotechnology. She was previously a health columnist for the Boston Globe and has contributed to Newsweek, Scientific American, and Nature, among others. She is the co-author of a college biology textbook, “Biology Now,” published by W.W. Norton. Megan received an M.S. from the Graduate Program in Science Writing at the Massachusetts Institute of Technology, a B.A. at Boston College, and worked as an educator at the Museum of Science, Boston.